Medical disclaimer: This article is for informational purposes only and does not replace professional medical advice. Talk to your doctor before starting any supplement, especially if you take prescription medications or have underlying health conditions.
The best vitamins for sciatica and nerve regeneration are B1 (benfotiamine), B6, B12 (methylcobalamin), alpha-lipoic acid (ALA), and acetyl-L-carnitine (ALC). Each of these targets a different part of nerve repair, from rebuilding the myelin sheath to reducing oxidative damage along the nerve pathway. I’ve spent years reviewing the clinical literature on neuropathy vitamins, and the evidence for these five is stronger than most people realize.
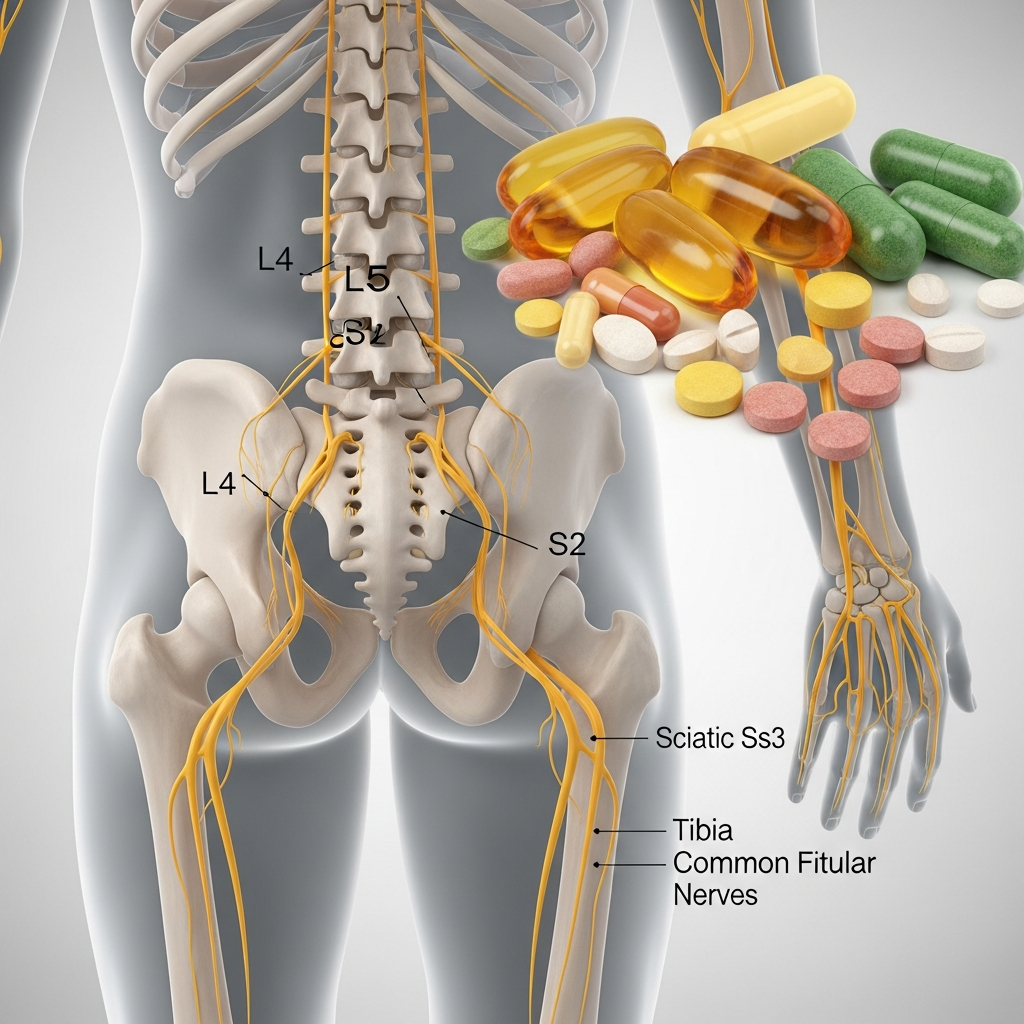
Sciatica affects roughly 40% of adults at some point in their lives, according to Harvard Health Publishing. The pain shoots from your lower back down through the buttock and leg, following the path of the sciatic nerve, the longest nerve in the human body. It originates from the L4 through S3 nerve roots in the lumbar spine. And while most cases resolve within 6 to 12 weeks, chronic sciatica can persist for months or years when the underlying nerve compression or inflammation goes unaddressed.
So what actually helps nerves heal? The answer is a combination of targeted nutrition, specific supplements backed by clinical trials, and consistent physical rehabilitation. Here’s what the research shows.
What Causes Sciatica (and Why Nerve Health Matters)
Sciatica happens when something compresses or irritates the sciatic nerve roots. The most common cause is a herniated disc in the lumbar spine, which accounts for about 90% of cases. Other causes include spinal stenosis (narrowing of the spinal canal), degenerative disc disease, spondylolisthesis (vertebral slippage), and piriformis syndrome (where the piriformis muscle in the buttock spasms and pinches the nerve).
The compression itself causes pain. But the real damage happens at the cellular level. When a nerve is compressed, blood flow decreases, oxygen supply drops, and inflammatory chemicals flood the area. Over time, the myelin sheath (the protective coating around the nerve fiber) can break down. Signal transmission slows. Numbness, tingling, and weakness follow.
This is where vitamins and supplements enter the picture. They don’t fix a herniated disc. But they can support the biological processes that repair nerve fibers, rebuild myelin, and reduce the inflammatory cascade that keeps the pain cycle going.
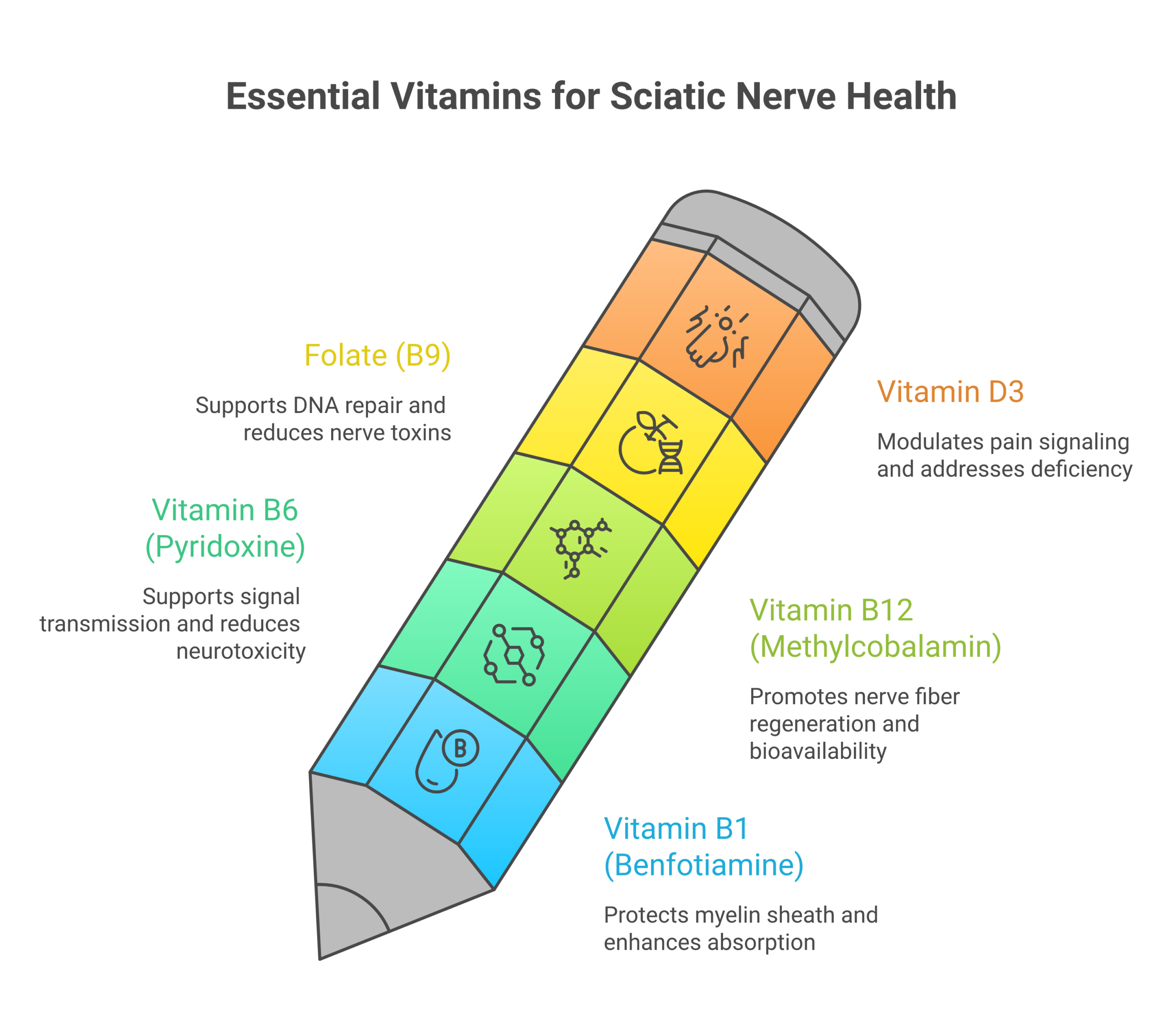
B Vitamins: The Foundation of Nerve Repair
B vitamins are the single most studied nutrient group for nerve health. A 2021 review published in BioMed Research International by researcher Simone Baltrusch analyzed 15 experimental animal studies documenting the nerve-regenerating effects of B vitamins, particularly B12. The evidence is clear: B1, B6, and B12 each support different aspects of nerve function, and they work better together than alone.
Vitamin B1 (Benfotiamine)
Regular thiamine (vitamin B1) is water-soluble and poorly absorbed. Benfotiamine is a fat-soluble form with roughly five times the bioavailability. In a study by Stracke et al. (2001), benfotiamine blocked the formation of advanced glycation end-products (AGEs), which are toxic compounds that damage nerve tissue. This is especially relevant for people with diabetes, but AGE accumulation also occurs with aging and high-sugar diets.
Benfotiamine protects the myelin sheath. It also supports glucose metabolism in nerve cells, which matters because nerves are extremely energy-hungry tissue. A typical dose in clinical studies is 150 to 300 mg per day.
Vitamin B6 (Pyridoxine)
B6 supports neurotransmitter synthesis and nerve signal transmission. Yang (2009) found that vitamin B6 inhibited neurotoxic glutamate release by suppressing calcium entry and protein kinase C activity in rat nerve terminals. Glutamate excitotoxicity is one of the mechanisms that worsens nerve damage after compression injuries.
Clinical data from carpal tunnel syndrome patients showed that B6 treatment increased sensory nerve conduction velocity. A word of caution: high-dose B6 (above 200 mg per day for extended periods) can itself cause peripheral neuropathy. Stick to 25 to 100 mg daily.
Vitamin B12 (Methylcobalamin)
B12 is the most important single vitamin for nerve regeneration. I’m not hedging on this. The research base is large and consistent.
Gan et al. (2014) demonstrated that high-dose vitamin B12 promoted dose-dependent increases in myelin thickness in mice after sciatic nerve injury. Tamaddonfard et al. (2014) found that B12 increased functional recovery and reduced Wallerian degeneration (the breakdown of nerve fibers after injury) in tibial nerve crush injuries. And Watanabe et al. (1994) showed that ultra-high dose methylcobalamin increased nerve fiber density in neuropathy models.
The form matters. Methylcobalamin is the active, bioavailable form. Cyanocobalamin (the cheaper, synthetic version) requires conversion in the body and delivers less of the vitamin to nerve tissue. Clinical doses range from 500 to 1,500 mcg per day for nerve support, with some studies using injectable doses of 1,000 mcg.
If you’re evaluating a nerve supplement, methylcobalamin (not cyanocobalamin) should be the B12 form listed on the label.
Folate (Vitamin B9)
Folate works with B12 to reduce homocysteine, an amino acid that at elevated levels is toxic to nerve cells. It also supports DNA repair in damaged neurons. Most adults need 400 to 800 mcg daily. Methylfolate (5-MTHF) is the bioactive form, preferred over folic acid for people with MTHFR gene variants.
Alpha-Lipoic Acid (ALA): The Antioxidant Nerve Protector
Alpha-lipoic acid is both water-soluble and fat-soluble, which means it can cross the blood-nerve barrier and work directly inside nerve cells. Its primary role is as an antioxidant, neutralizing the reactive oxygen species that accumulate in compressed or inflamed nerves.
A 2023 randomized controlled trial by Scaturro et al., published in Medicina, studied 128 young adults with discogenic sciatica. Patients who received 600 mg of ALA daily (combined with rehabilitation and other supplements) saw their pain scores drop from 6.4 to 3.2 on a 10-point scale at 60 days. The rehabilitation-only group dropped from 6.2 to 4.1. The supplement-only group dropped from 6.3 to 4.8. The combination group outperformed both individual approaches.
ALA has also been studied for diabetic neuropathy. A review published in Nutrients (2020) analyzed its efficacy for nerve conduction velocity and found significant improvements compared to placebo.
Standard dosing is 600 mg per day. Some practitioners recommend the R-lipoic acid form for better absorption, though most clinical trials used racemic ALA (the 50/50 R/S mixture).
Acetyl-L-Carnitine (ALC): Proven Nerve Regenerator
If there’s one supplement on this list with the strongest direct evidence for nerve regeneration, it’s acetyl-L-carnitine. And I mean actual regeneration: new nerve fiber growth measured under a microscope.
Sima, Calvani, Mehra, and Amato published a landmark analysis in Diabetes Care (2005) combining data from two 52-week randomized, placebo-controlled trials with 1,257 patients. At a dose of 1,000 mg three times daily, ALC produced significant improvements in sural nerve fiber numbers and regenerating nerve fiber clusters. It also improved pain scores and vibratory perception. The pain reduction was statistically significant in the combined cohort.
ALC works through multiple mechanisms. It promotes DNA synthesis in mitochondria, increases nerve growth factor (NGF) concentrations in neurons, reduces oxidative stress, and directly supports axonal regrowth. Peripheral nerves regenerate at roughly 1 mm per day (about 1 inch per month), according to data from Ochsner Journal, and ALC appears to support this process.
Doses in clinical trials ranged from 1,500 to 3,000 mg per day, divided into two or three doses. It’s generally well-tolerated, with mild gastrointestinal upset being the most common side effect.
PEA (Palmitoylethanolamide): The Pain Reducer
PEA is a fatty acid amide produced naturally in the body during tissue damage and inflammation. It works through the endocannabinoid system (without being a cannabinoid) and targets mast cells and glial cells that drive neuropathic pain.
The strongest sciatica-specific evidence comes from a double-blind, placebo-controlled trial by Guida et al. (2010) involving 636 patients with sciatic nerve compression. At 600 mg per day, pain scores dropped from 7.1 to 2.1 on the visual analog scale after just three weeks. The placebo group dropped from 6.6 to 4.6. The number needed to treat (NNT) to achieve 50% pain reduction was 1.5, which is exceptionally strong for any pain intervention.
A 2023 meta-analysis in Nutrients confirmed PEA’s efficacy for chronic pain across multiple conditions, with a favorable safety profile and no documented drug interactions. Micronized PEA (micro-PEA) appears to have better bioavailability than standard forms.
If you’re dealing with active sciatic pain and want fast relief while working on long-term nerve repair, PEA at 600 mg per day is worth discussing with your doctor. For more background on supplement safety, see our guide on whether nerve supplements are safe.
Vitamin D3: The Overlooked Nerve Nutrient
Vitamin D receptors have been identified in the spinal cord, nerve roots, dorsal root ganglia, and glial cells. A 2021 animal study published in Pharmacological Reports found that vitamin D3 supplementation (500 IU/kg per day) significantly reduced nociception markers in a rat model of neuropathic pain. The vitamin also showed antioxidant activity in spinal cord tissue.
In a study of 145 patients with chronic low back and leg pain (published in Acta Orthopaedica et Traumatologica Turcica), 22.8% had outright vitamin D deficiency and another 42.8% had insufficiency. That’s nearly two-thirds of chronic pain patients with suboptimal vitamin D levels.
Vitamin D deficiency is extremely common in adults over 50, people who live in northern latitudes, and anyone who spends most of their time indoors. A blood test (25-hydroxy vitamin D) is the only way to know your level. Target 40 to 60 ng/mL for optimal nerve and bone health. Most people need 2,000 to 5,000 IU of D3 daily to reach this range, though your doctor should guide the dose based on your bloodwork.
Curcumin: Anti-Inflammatory Support
Curcumin (the active compound in turmeric) reduces NF-kB, a key inflammatory signaling molecule involved in nerve pain. Standard curcumin has very poor bioavailability. You need a formulation with enhanced absorption, such as curcumin combined with piperine, or a phytosomal form like Meriva.
The evidence for curcumin in neuropathy is mostly preclinical, but it consistently shows reduced inflammation and oxidative damage in nerve tissue. I include it here as a supporting supplement rather than a primary one. Doses of 500 to 1,000 mg of enhanced-bioavailability curcumin per day are typical.
How Nerve Regeneration Actually Works
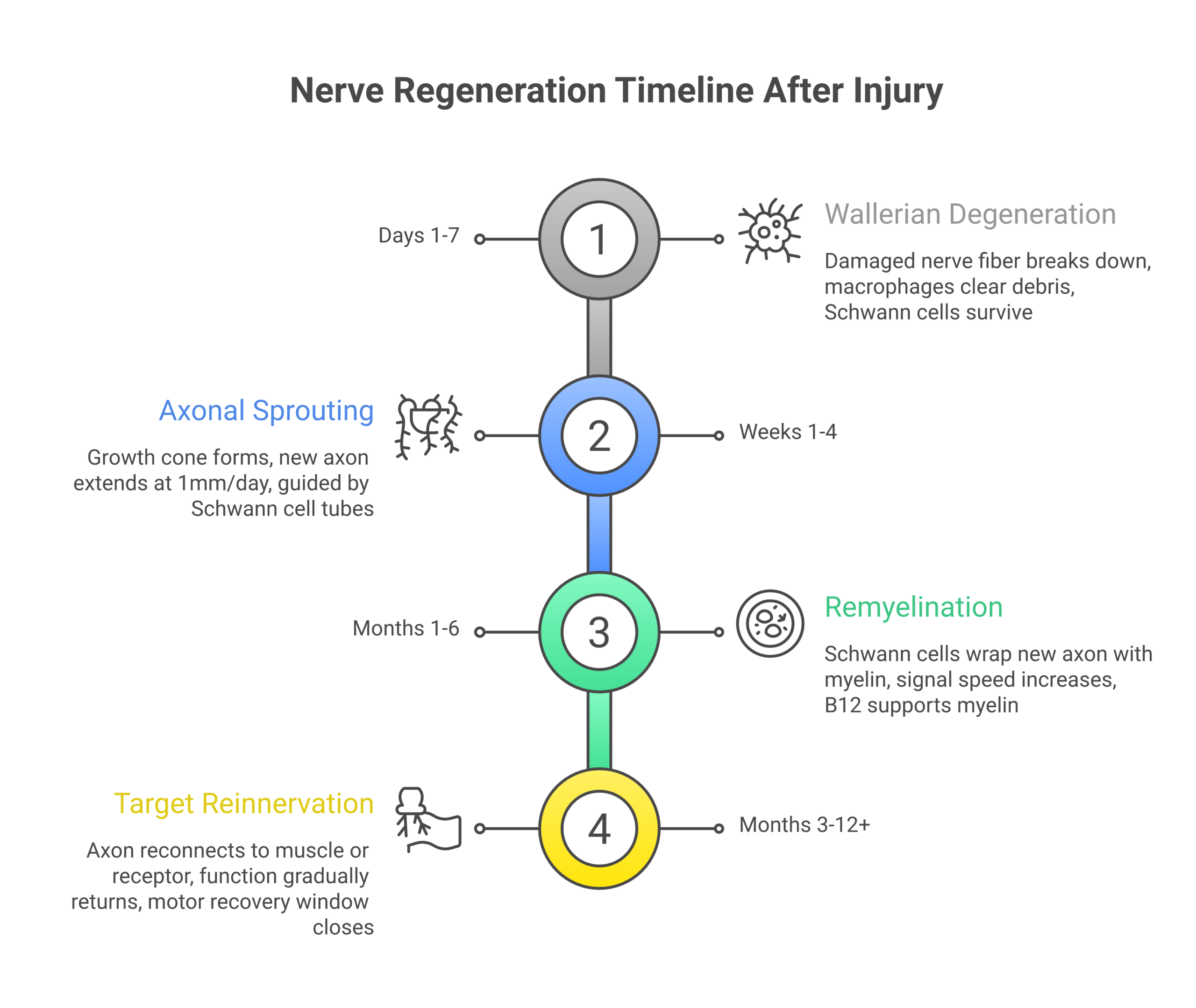
Understanding the biology helps you set realistic expectations. After a nerve is damaged, recovery happens in four phases.
Phase 1, Wallerian degeneration (days 1 to 7): The damaged nerve fiber breaks down beyond the point of injury. Macrophages move in to clear debris. Schwann cells (the cells that produce myelin) survive and form a tube-like pathway for the regrowing nerve.
Phase 2, axonal sprouting (weeks 1 to 4): A growth cone forms at the tip of the surviving nerve stump. The new axon extends through the Schwann cell pathway at approximately 1 mm per day.
Phase 3, remyelination (months 1 to 6): Schwann cells begin wrapping the new axon with myelin. Signal speed gradually increases. This is where B12 and benfotiamine are most active.
Phase 4, target reinnervation (months 3 to 12+): The axon reaches its target muscle or sensory receptor and forms a new connection. Motor end plates remain viable for reinnervation for roughly 12 to 16 months after denervation. After that window, permanent muscle atrophy can occur.
Supplements support phases 2 and 3 most directly. ALC and ALA support axonal sprouting and oxidative protection. B vitamins support remyelination. PEA manages pain throughout all four phases.
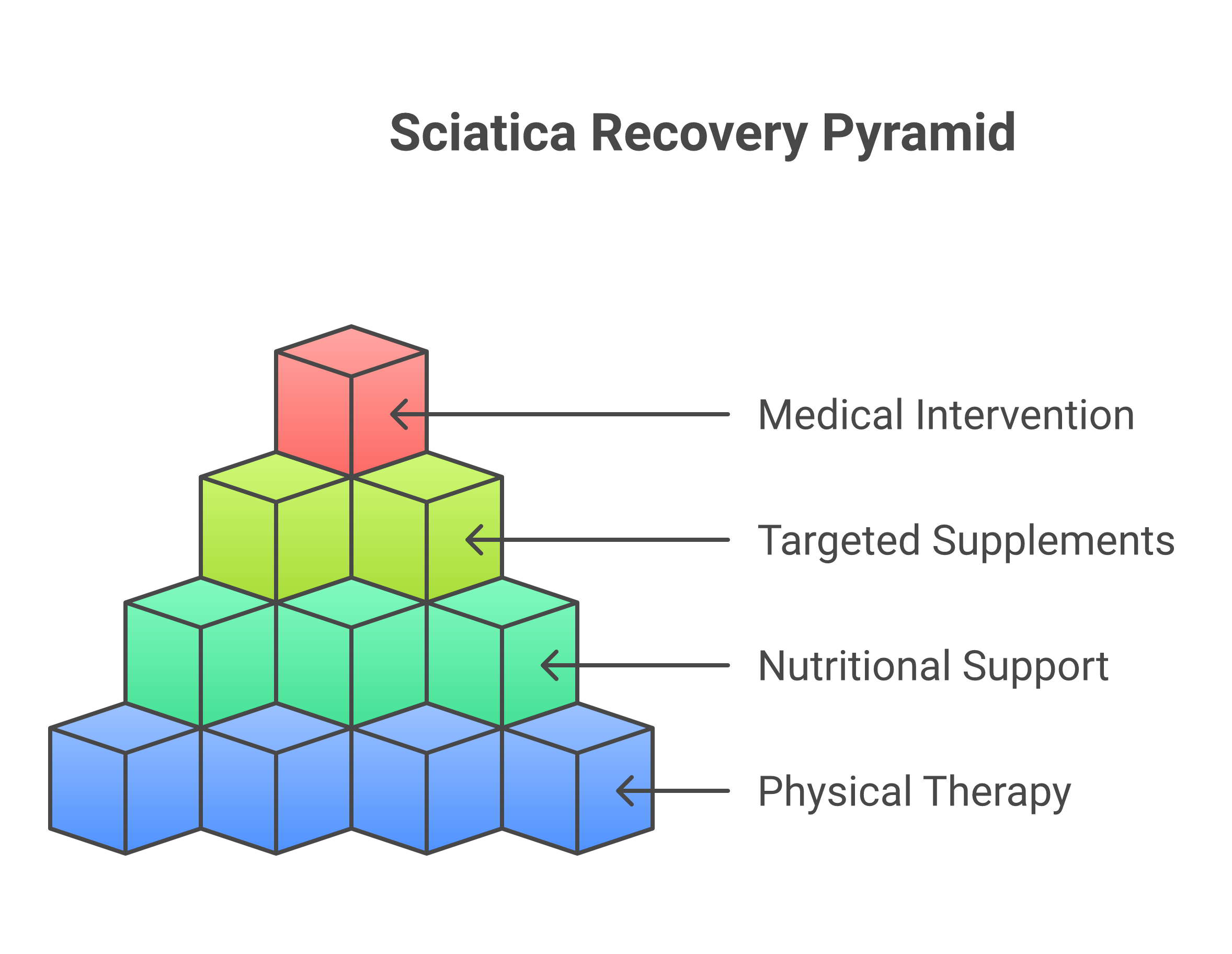
Lifestyle Factors That Help Nerves Heal
Supplements alone won’t fix sciatica. They work best alongside these evidence-based strategies.
Physical Therapy and Targeted Stretching
The McKenzie method, sciatic nerve flossing, and core stabilization exercises have the best evidence for sciatica relief. A physical therapist can identify which movements help and which ones aggravate your specific nerve compression pattern. Most sciatica guidelines recommend at least 6 weeks of physical therapy before considering invasive interventions.
Anti-Inflammatory Diet
Omega-3 fatty acids (from fatty fish, flaxseed, or supplementation at 2 to 3 grams of EPA/DHA per day) reduce systemic inflammation. Colorful vegetables provide polyphenols that protect nerve tissue. Processed foods, excess sugar, and seed oils promote inflammation. You don’t need a perfect diet, but shifting toward whole foods makes a measurable difference in inflammatory markers.
For more on how food choices affect nerve function, read our article on what foods are good for overactive nerves.
Walking
It sounds too simple. But regular walking increases blood flow to the nerve roots, promotes endorphin release, and prevents the deconditioning that makes chronic pain worse. Start with what you can tolerate (even 5 minutes), and build gradually to 30 minutes per day.
Sleep Quality
Nerve repair happens primarily during sleep. Growth hormone release peaks during deep sleep, and this hormone is directly involved in tissue repair. Poor sleep slows recovery. If pain disrupts your sleep, address this with your doctor early.
When Surgery Is Needed
Only 5% to 10% of sciatica cases require surgery, according to the American Academy of Orthopaedic Surgeons. Surgery is typically recommended when conservative treatment fails after 6 to 12 weeks, progressive neurological deficits develop (such as foot drop or bladder dysfunction), or an MRI shows severe nerve compression requiring decompression.
A microdiscectomy (removal of the herniated disc fragment pressing on the nerve) has a success rate of roughly 85% to 90% for leg pain relief. Recovery time is usually 4 to 6 weeks. Supplements can still support nerve recovery after surgery during the regeneration phase.
Putting It All Together: A Practical Supplement Stack
Based on the clinical evidence, here’s what a targeted supplement approach for sciatica and nerve regeneration looks like. Discuss this with your healthcare provider before starting.
- B-complex with active forms: B1 as benfotiamine (150 to 300 mg), B6 as pyridoxine (25 to 50 mg), B12 as methylcobalamin (1,000 to 1,500 mcg), folate as methylfolate (400 to 800 mcg)
- Alpha-lipoic acid: 600 mg daily
- Acetyl-L-carnitine: 1,500 to 3,000 mg daily, divided into 2 to 3 doses
- PEA (micronized): 600 mg daily for active pain
- Vitamin D3: 2,000 to 5,000 IU daily (based on blood levels)
- Curcumin (enhanced absorption): 500 to 1,000 mg daily (optional, for additional anti-inflammatory support)
This isn’t a random list. Every item on it has at least one published randomized controlled trial showing benefit for nerve-related outcomes. The B vitamins, ALC, and ALA have the deepest evidence base. PEA has the strongest data specifically for sciatic pain.
To find a quality product that includes many of these ingredients, see our verified nerve supplement reviews.
What to Expect: Realistic Timelines
Nerve regeneration is slow. Here’s what the research suggests for realistic expectations.
- Weeks 1 to 3: PEA may begin reducing pain. Anti-inflammatory effects from ALA and curcumin start building
- Weeks 4 to 8: B vitamin levels optimize. Early signs of improved sensation may appear in mild cases
- Months 2 to 6: Nerve fiber regeneration is measurable. Vibratory perception and numbness may begin improving
- Months 6 to 12: Significant functional recovery if the nerve was not severely damaged. The 1 mm per day regeneration rate means a nerve injured 6 inches from its target takes roughly 150 days to reconnect
Patience matters. Most people give up on supplements after 2 to 4 weeks, well before nerve regeneration has had time to occur. The clinical trials that showed benefit lasted 12 to 52 weeks. Commit to at least 3 months before evaluating results.
For help choosing the right product, check our guide on what to look for in a nerve supplement, and browse our independent nerve supplement reviews.
Frequently Asked Questions
What is the best vitamin for sciatic nerve pain?
Vitamin B12 in the methylcobalamin form has the most evidence for sciatic nerve support. A 2021 review in BioMed Research International documented 15 animal studies confirming B12’s nerve-regenerating effects, including dose-dependent increases in myelin thickness after sciatic nerve injury (Gan et al., 2014). For fastest pain relief specifically, PEA at 600 mg daily showed an NNT of 1.5 in a 636-patient trial.
Can damaged nerves actually regenerate?
Yes, peripheral nerves can regenerate, though the process is slow. Axons regrow at approximately 1 mm per day (about 1 inch per month). Schwann cells form a pathway that guides regrowth, and remyelination follows over several months. The critical window for motor nerve reconnection is 12 to 16 months after injury. Supplements like ALC and B12 support this process, as documented in the Sima et al. (2005) study in Diabetes Care.
How long does it take for sciatica to heal with supplements?
Most clinical trials showing benefit for nerve supplements lasted 12 to 52 weeks. PEA can reduce pain within 3 weeks, based on the Guida et al. (2010) trial. Nerve fiber regeneration (measured by ALC studies) takes 6 to 12 months. Mild sciatica may resolve faster. Set a minimum evaluation period of 3 months before deciding whether supplements are helping.
Are nerve supplements safe to take long-term?
B vitamins, ALA, ALC, and PEA all have favorable long-term safety profiles in clinical trials lasting up to 52 weeks. The main caution is vitamin B6: doses above 200 mg per day for extended periods can cause neuropathy. ALC’s most common side effect is mild GI upset. PEA had zero documented drug interactions in the Guida trial with 636 patients. Always tell your doctor what supplements you take, especially if you’re on blood thinners or diabetes medications. Learn more in our nerve supplement safety guide.
Does vitamin D help with sciatica?
Vitamin D receptors exist in the spinal cord, nerve roots, and dorsal root ganglia. A study of 145 chronic low back and leg pain patients found 65% had deficient or insufficient vitamin D levels. Animal research (2021, Pharmacological Reports) showed D3 supplementation reduced neuropathic pain markers. While D alone likely won’t resolve sciatica, correcting a deficiency removes a barrier to nerve healing. Get your levels tested, target 40 to 60 ng/mL.
What is the difference between benfotiamine and regular vitamin B1?
Benfotiamine is a fat-soluble form of vitamin B1 with roughly five times the bioavailability of regular thiamine. Because it’s fat-soluble, it can cross cell membranes more easily and reach nerve tissue at higher concentrations. Stracke et al. (2001) showed benfotiamine was more effective than water-soluble thiamine at blocking AGE formation, which damages nerves. Most quality nerve supplements use benfotiamine rather than standard thiamine.
Should I take all these supplements together?
The combination approach has direct clinical support. Jolivalt et al. (2009) found that combining B1, B6, and B12 restored sensory nerve function more effectively than any single B vitamin alone. Scaturro et al. (2023) showed that combining ALA, ALC, and vitamin D with rehabilitation outperformed either approach used individually. Start with the B vitamins and add one supplement at a time so you can identify what helps and what causes any side effects.
For more resources on nerve health, visit our nerve supplement category, read about foods that support nerve health, or learn more about our review process.