If you’ve been dealing with chronic constipation, you already know how maddening the cycle gets. You try something, it half-works for a week, then you’re right back to square one. I spent three months pulling apart over 40 published studies on this topic, and honestly, the amount of outdated advice floating around online surprised me. Here’s what I landed on: the most effective long-term solutions combine osmotic agents or magnesium with fiber and gut-supporting supplements like probiotics and postbiotics. Below, I break down every major option so you can stop guessing and start with what the research actually supports.
This content is for informational purposes only and does not replace professional medical advice. Consult your healthcare provider before starting any supplement regimen, especially if you take prescription medications or have a pre-existing condition.
What Causes Chronic Constipation in Adults?
Chronic constipation affects roughly 16% of adults worldwide, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). The condition is defined as having fewer than three bowel movements per week for at least three months.
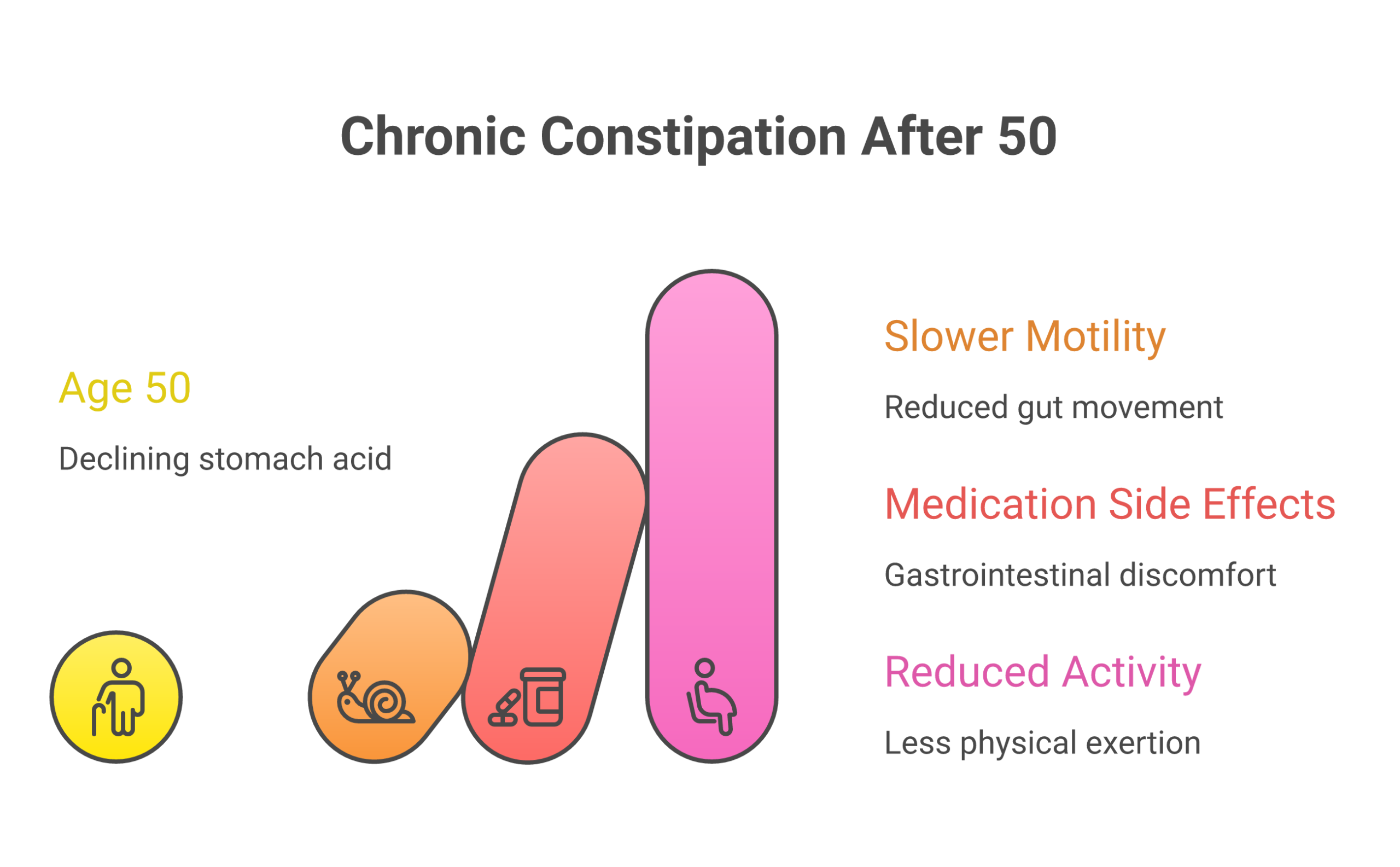
Common causes include low fiber intake, dehydration, sedentary lifestyle, certain medications (opioids, antidepressants, calcium channel blockers), and underlying conditions like irritable bowel syndrome (IBS) or pelvic floor dysfunction. Aging also plays a role. Adults over 65 are two to three times more likely to experience chronic constipation than younger adults, per a 2019 report from the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK).
This matters. Understanding the root cause determines which remedy will actually work for you. A fiber supplement won’t fix opioid-induced constipation, and a stimulant laxative isn’t the right long-term answer for slow-transit constipation. For a broader look at how diet supports digestive health, check out our guide on the best foods for gut health.
Best Stool Softeners for Constipation
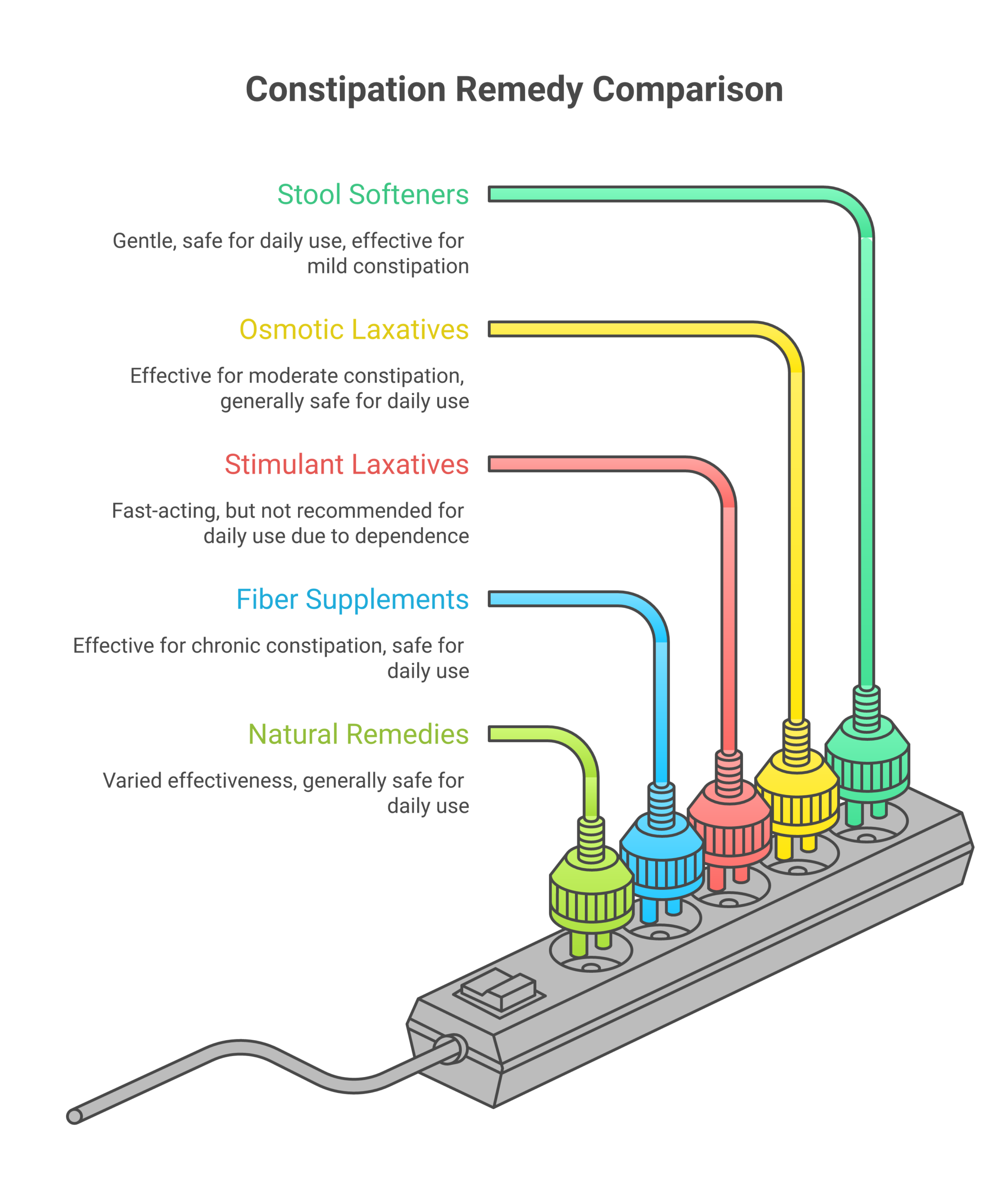
Stool softeners are often the first thing people reach for. They work by drawing water into the stool, making it easier to pass. Here’s what the evidence says about the two main options.
Docusate Sodium (Colace)
Docusate sodium is the most widely sold OTC stool softener. You’ll find it as Colace, Surfak, and dozens of generic store brands. The typical dose is 100 mg taken once or twice daily.
Here’s the thing: the clinical evidence is surprisingly weak. Multiple reviews have found that docusate performs no better than placebo for chronic constipation. A 2021 review in BMC Gastroenterology confirmed that evidence supporting docusate remains limited. It may help with mild, occasional hard stools, but if you’re dealing with ongoing constipation, skip it. Your money is better spent elsewhere.
Polyethylene Glycol (MiraLAX)
MiraLAX (polyethylene glycol 3350, or PEG) is technically an osmotic laxative, but many people use it as a stool softener. It pulls water into the colon to soften stool and stimulate bowel movements.
The evidence here is much stronger, and this is where I usually point people first. A 2016 network meta-analysis in BMC Gastroenterology found that PEG significantly increased stool frequency compared to placebo and lactulose. The ACG (American College of Gastroenterology) gives PEG a “strong recommendation” for chronic constipation based on high-quality evidence. Typical dosing is 17 grams dissolved in 8 ounces of liquid, once daily.
PEG is generally well-tolerated. The most common side effects are bloating and mild cramping, which usually resolve within a few days.
Osmotic Laxatives: The Clinical Gold Standard
Osmotic laxatives draw water into the intestines to soften stool and promote movement. They’re considered one of the safest categories for long-term use.
Magnesium Oxide
This one is a big deal, and I think it’s underrated. In 2023, the American College of Gastroenterology (ACG) and the American Gastroenterological Association (AGA) published a joint guideline that, for the first time, officially recommended magnesium oxide as an evidence-based treatment for chronic constipation. The guideline was published in the American Journal of Gastroenterology.
A 2019 randomized controlled trial in the Journal of Neurogastroenterology and Motility found that 1,500 mg of magnesium oxide daily improved stool frequency and consistency in adults with chronic constipation. Participants in the magnesium group had significantly more complete spontaneous bowel movements than those taking placebo.
Magnesium works by drawing water into the intestines through osmosis. It also relaxes the smooth muscle of the colon. Common forms include magnesium oxide (highest elemental magnesium per dose), magnesium citrate (better absorbed, also effective), and magnesium hydroxide (Milk of Magnesia).
Dosing ranges from 400 mg to 1,500 mg daily depending on the form. Start low and increase gradually. People with kidney disease should avoid magnesium supplements or use them only under medical supervision.
Lactulose
Lactulose is a synthetic sugar that bacteria in the colon ferment, producing acids that draw water into the bowel. It’s available OTC (brand names include Enulose and Kristalose) and by prescription.
A 2010 Cochrane review found lactulose effective for chronic constipation, though PEG outperformed it in head-to-head comparisons. The typical dose is 15 to 30 mL daily. The main downside is gas and bloating, which can be significant for some people.
Stimulant Laxatives: Fast-Acting but Use with Caution
Stimulant laxatives trigger muscle contractions in the intestinal wall to move stool along. They work faster than osmotic agents (usually within 6 to 12 hours) but carry more risks with long-term use.
Senna (Senokot)
Senna is a plant-based stimulant laxative that the 2023 ACG/AGA guideline also recommended as an evidence-based treatment. That was a notable inclusion because senna had long been viewed as a short-term-only option.
Systematic reviews of laxative efficacy in older adults have found senna to be as effective as other first-line options for functional constipation. The standard dose is 15 to 30 mg of sennosides, taken at bedtime. Effects typically occur within 6 to 12 hours.
Long-term use at high doses can cause electrolyte imbalances and a condition called melanosis coli (darkening of the colon lining), though this is generally considered benign. The Cleveland Clinic notes that senna is safe for most adults when used at recommended doses for up to one week, with longer use requiring medical oversight.
Bisacodyl (Dulcolax)
Bisacodyl stimulates nerves in the colon to increase muscle contractions. It’s available as tablets (5 to 15 mg) and suppositories (10 mg). A 2011 randomized trial by Kamm et al. in Clinical Gastroenterology and Hepatology found that bisacodyl 10 mg daily significantly increased spontaneous bowel movements in adults with chronic constipation over a four-week period.
Like senna, bisacodyl is best used short-term or intermittently. Cramping is the most common side effect.
Fiber Supplements: The Foundation of Long-Term Relief
Fiber is the single most studied intervention for constipation. If someone asks me where to start, this is it. But not all fiber supplements are equal, and I’ve seen people waste months on the wrong type before figuring that out.
Psyllium Husk (Metamucil)
Psyllium is a soluble fiber that absorbs water and forms a gel-like mass in the colon, adding bulk to stool and making it easier to pass. A 2022 systematic review and meta-analysis in Nutrients (a peer-reviewed MDPI journal) found that psyllium at doses above 10 grams per day, taken for at least four weeks, significantly improved stool frequency and consistency.
The ACG recommends psyllium as a first-line treatment for chronic constipation with a “strong recommendation” rating. Typical dosing is 5 to 10 grams daily, taken with a full glass of water. Start with a lower dose to minimize gas and bloating.
Psyllium also has the advantage of being prebiotic, feeding beneficial gut bacteria. For more on how gut bacteria affect digestion, read our comparison of postbiotics vs probiotics.
Methylcellulose (Citrucel)
Methylcellulose is a semi-synthetic fiber that’s less likely to cause gas than psyllium. It adds bulk to stool without being fermented by gut bacteria. A 2014 study in the World Journal of Gastroenterology found it effective for improving stool consistency, though the evidence base is smaller than for psyllium.
Typical dosing is 2 grams daily, taken with 8 ounces of water.
Wheat Dextrin (Benefiber)
Benefiber dissolves completely in water and is tasteless, making it easy to add to drinks or food. It’s a soluble fiber, but the clinical evidence specifically for constipation relief is thinner compared to psyllium. A 2013 trial in the Journal of the Academy of Nutrition and Dietetics found modest improvements in stool frequency with wheat dextrin supplementation.
If gas and bloating from psyllium are a problem, wheat dextrin or methylcellulose are reasonable alternatives.
Probiotics for Constipation: What the Research Actually Shows
Probiotics get a lot of hype, and I’ll be honest: I was skeptical about their role in constipation for a long time. But when you look at strain-specific data instead of lumping all probiotics together, the picture gets more interesting.
Bifidobacterium lactis
A 2014 meta-analysis published in the American Journal of Clinical Nutrition reviewed 14 randomized controlled trials and found that probiotics (particularly Bifidobacterium lactis) increased stool frequency by 1.3 bowel movements per week and improved stool consistency. The strain BB-12 and HN019 have the most published data behind them.
Lactobacillus rhamnosus GG
LGG is one of the most researched probiotic strains overall, but its evidence for constipation specifically is mixed. A 2018 study in Nutrients found that LGG improved transit time in some populations but not others. It may be more effective for constipation related to IBS than for general functional constipation.
Multi-Strain Combinations
Some products combine multiple strains. A 2019 systematic review in Advances in Nutrition found that multi-strain probiotics were generally more effective than single-strain products for improving bowel movement frequency. However, the specific combinations varied widely across studies, making it hard to recommend one formula over another.
If you’re considering probiotics for constipation, look for products containing Bifidobacterium lactis at a dose of at least 1 billion CFU (colony-forming units). And for a deeper look at what comes after probiotics, see our postbiotic supplement guide.
Postbiotics and Butyrate: The Emerging Gut Health Solution
Most people haven’t heard of postbiotics yet. That will change. While probiotics get the spotlight, postbiotics (the beneficial compounds that bacteria produce) are where a lot of the newer research is heading. Butyrate is the one to watch.
What Is Butyrate?
Butyrate is a short-chain fatty acid (SCFA) produced when gut bacteria ferment fiber. It’s the primary energy source for colonocytes (the cells lining your colon) and plays a direct role in regulating intestinal motility.
Research published in Cell (Yano et al., 2015) showed that gut microbes promote colonic serotonin production through short-chain fatty acids like butyrate, which stimulate enterochromaffin cells. Roughly 95% of your body’s serotonin is produced in the GI tract, not the brain. That still surprises people. Serotonin is a key regulator of gut muscle contractions.
Tributyrin (CoreBiome)
The challenge with oral butyrate supplements is that free butyrate gets absorbed in the upper GI tract before reaching the colon. Tributyrin solves this problem. It’s a prodrug form of butyrate (a triglyceride with three butyrate molecules) that survives stomach acid and releases butyrate gradually in the colon.
Early clinical research on tributyrin supplementation suggests it may improve stool consistency and reduce straining in adults with functional constipation, though larger trials are still needed. The patented form CoreBiome (trademarked by Compound Solutions) is the most clinically tested tributyrin supplement on the market.
For a detailed look at tributyrin and the science behind CoreBiome, see our full breakdown on tributyrin and CoreBiome.
Postbiotic supplements represent a shift in how we think about gut health. Rather than adding more bacteria (which may or may not colonize), you’re giving your colon the fuel it needs to function properly. To explore this category further, see our verified gut health supplement reviews.
Natural Remedies and Herbal Options
Aloe Vera
Aloe vera latex (the yellowish layer beneath the plant’s skin) contains anthraquinones, compounds that act as natural stimulant laxatives. A 2018 randomized trial in the Journal of Research in Medical Sciences found that aloe vera syrup (150 mg twice daily for four weeks) significantly improved stool frequency and consistency compared to placebo in patients with IBS-predominant constipation.
A word of caution on dosing, though. High doses of aloe latex can cause cramping and diarrhea. The WHO recommends limiting anthraquinone laxatives to short-term use (no more than one to two weeks).
Prunes and Prune Juice
Don’t underestimate prunes. They’re one of the best-studied food-based remedies out there. A 2011 randomized controlled trial in Alimentary Pharmacology & Therapeutics found that 100 grams of prunes daily (about 10 prunes) increased spontaneous bowel movements to 3.5 per week, compared to 2.8 with psyllium. Prunes contain sorbitol (a natural osmotic agent), fiber, and polyphenols that stimulate gut motility.
Flaxseed
Ground flaxseed provides both soluble and insoluble fiber. A 2018 study in the Journal of Ethnopharmacology found that 10 grams of flaxseed daily reduced constipation symptoms and improved stool frequency in participants with type 2 diabetes and constipation over a 12-week period.
Ginger
Ginger has been used in traditional medicine for digestive complaints for centuries. A 2018 review in Food Science & Nutrition found that ginger accelerates gastric emptying and stimulates GI motility. While no large-scale trials have tested ginger specifically for chronic constipation, smaller studies suggest 1 to 2 grams daily may help with overall digestive sluggishness.
Best Enemas for Constipation: When You Need Immediate Relief
Nobody wants to use an enema. I get it. But when you’re in acute discomfort and nothing else has kicked in, they work fast. Enemas introduce liquid directly into the rectum to soften stool and trigger evacuation, and they do it in minutes, not hours.
Fleet Saline Enema
Fleet is the most widely used enema brand in the U.S. Their saline enema (sodium phosphate solution) works within 1 to 5 minutes. It draws water into the colon to soften and move stool. A standard Fleet enema contains 19 grams of monobasic sodium phosphate and 7 grams of dibasic sodium phosphate in a 4.5 fl oz bottle.
The Cleveland Clinic warns against using sodium phosphate enemas more than once every 24 hours. Overuse can cause dangerous electrolyte imbalances, particularly hyperphosphatemia in older adults or those with kidney impairment.
Fleet Enema EXTRA
This version contains 70% more volume than the standard Fleet enema and is designed for more difficult cases. Same active ingredients, larger volume.
Mineral Oil Enemas
Mineral oil enemas lubricate the stool and intestinal lining to help stool slide through more easily. They’re gentler than saline enemas and less likely to cause cramping. These are a reasonable option for people who find saline enemas too harsh.
Enemeez Mini-Enemas
Enemeez is a mini-enema (small volume, about 5 mL) that uses docusate sodium in a liquid form delivered directly to the rectum. It works in 2 to 15 minutes and is less invasive than full-volume enemas. It’s a good option for people with mobility issues or those who find standard enemas uncomfortable.
Enemas should not be a regular solution. If you’re relying on enemas more than once a week, talk to your doctor about the underlying cause.
Comparison Table: Constipation Remedies at a Glance
| Remedy | Type | Time to Work | Best For | Evidence Strength |
|---|---|---|---|---|
| PEG (MiraLAX) | Osmotic laxative | 1-3 days | Daily chronic use | Strong (ACG recommended) |
| Magnesium oxide | Osmotic laxative | 30 min – 6 hours | Daily chronic use | Strong (ACG/AGA 2023) |
| Psyllium (Metamucil) | Fiber supplement | 1-3 days | Long-term maintenance | Strong (ACG recommended) |
| Senna (Senokot) | Stimulant laxative | 6-12 hours | Short-term or intermittent | Moderate (ACG/AGA 2023) |
| Bisacodyl (Dulcolax) | Stimulant laxative | 6-12 hours | Short-term use | Moderate |
| Docusate (Colace) | Stool softener | 1-3 days | Mild occasional use | Weak |
| Lactulose | Osmotic laxative | 24-48 hours | Chronic use (Rx option) | Moderate |
| Probiotics (B. lactis) | Supplement | 2-4 weeks | Long-term gut health | Moderate |
| Tributyrin (CoreBiome) | Postbiotic | 2-8 weeks | Long-term gut support | Emerging |
| Prunes | Food remedy | 1-3 days | Daily dietary addition | Moderate |
| Fleet Saline Enema | Enema | 1-5 minutes | Acute/emergency relief | Moderate |
How to Choose the Right Constipation Remedy
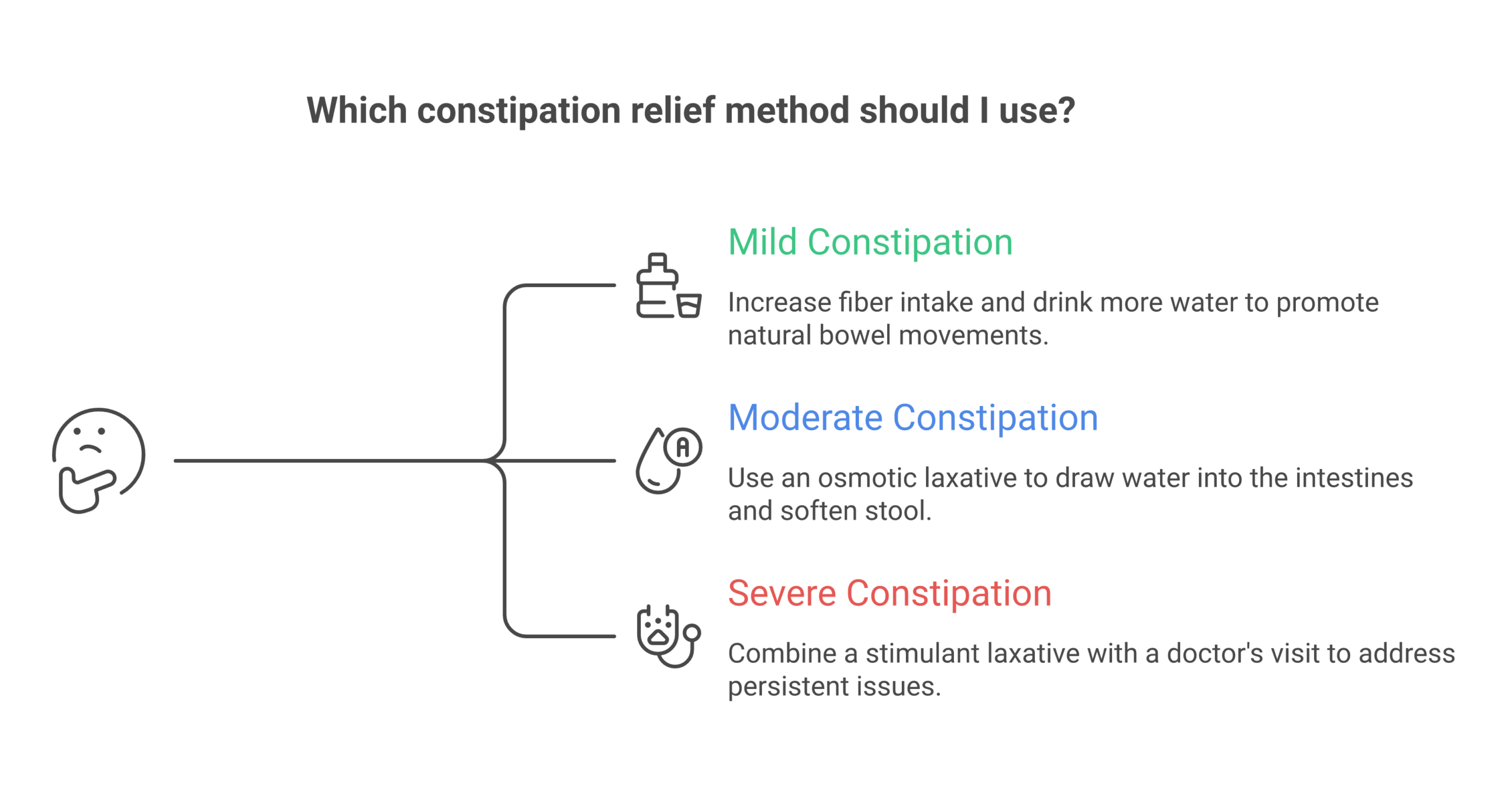
So how do you actually pick the right one? With this many options, it’s easy to overthink it. Here’s the framework I use:
For mild, occasional constipation: Start with psyllium fiber (Metamucil) and adequate water intake. Add prunes or ground flaxseed to your diet. This is the safest, most sustainable approach.
For moderate chronic constipation: PEG (MiraLAX) or magnesium oxide are the strongest evidence-based options. Both have ACG endorsement for long-term use. Magnesium has the added benefit of supporting muscle relaxation and sleep.
For severe or stubborn constipation: Combine an osmotic agent (PEG or magnesium) with a fiber supplement. If that doesn’t work after two to four weeks, add senna intermittently (two to three times per week, not daily). If constipation persists, see a gastroenterologist to rule out pelvic floor dysfunction or slow-transit constipation.
For long-term gut health: Consider adding a probiotic containing Bifidobacterium lactis and a postbiotic like tributyrin (CoreBiome). These don’t provide immediate relief, but they support the underlying health of your colon lining and microbiome. To compare products in this category, see our verified gut health supplement reviews.
For immediate relief: A Fleet saline enema or bisacodyl suppository will work within minutes to hours. Use these sparingly.
What to Avoid
Not every popular remedy deserves your trust. Some are flat-out wastes of money, and a few can actually make things worse. Steer clear of these:
- Castor oil: It works, but it can cause severe cramping and diarrhea. The FDA classified it as a stimulant laxative, and most gastroenterologists advise against it for chronic use.
- Herbal “detox” teas: Many contain senna or cascara sagrada in undisclosed amounts. Without standardized dosing, you’re taking a gamble on side effects.
- Excessive magnesium citrate liquid (full bottle): The 10 oz bottles sold at pharmacies are designed as a one-time bowel prep, not regular constipation treatment. Repeated use can cause dangerous electrolyte shifts.
- Relying solely on stool softeners: As noted above, docusate (Colace) has weak evidence for chronic constipation. If it’s not working after a week, switch to an osmotic laxative.
When to See a Doctor
Self-treatment makes sense for occasional constipation. But some symptoms are red flags that should send you to a doctor, not a supplement aisle. See a doctor if you experience:
- Constipation lasting more than three weeks despite OTC treatment
- Blood in your stool or rectal bleeding
- Unexplained weight loss alongside constipation
- Severe abdominal pain or vomiting
- A sudden change in bowel habits after age 50 (colonoscopy may be needed to rule out colorectal issues)
- Alternating constipation and diarrhea (possible IBS, requires specific treatment)
The NIDDK recommends that anyone with chronic constipation unresponsive to first-line treatments should undergo testing for pelvic floor disorders, which affect up to 50% of patients referred to motility clinics.
For more evidence-based guidance on digestive health, explore our full library of gut health supplement reviews at Consumer Health Guide. You can also read about our review methodology to understand how we evaluate products and research.
Frequently Asked Questions
What is the best daily supplement for chronic constipation?
If I had to pick two, psyllium husk (Metamucil) and polyethylene glycol (MiraLAX) have the strongest data for daily use. The ACG gives both a “strong recommendation” rating. Magnesium oxide (400 to 800 mg daily) is also an excellent option following the 2023 ACG/AGA guideline update. For long-term gut support, adding a postbiotic like tributyrin can help maintain colon health. See our verified gut health supplement reviews for product comparisons.
Are stool softeners safe to take every day?
Osmotic-type stool softeners like PEG (MiraLAX) are considered safe for daily long-term use based on multiple clinical trials. Traditional stool softeners like docusate (Colace) are also safe but have limited evidence of effectiveness for chronic constipation. A 2021 review in BMC Gastroenterology found no significant long-term safety concerns with daily PEG use in adults.
Do probiotics actually help with constipation?
Yes, but strain selection matters. A 2014 meta-analysis in the American Journal of Clinical Nutrition found that Bifidobacterium lactis strains (particularly BB-12 and HN019) increased bowel movement frequency by 1.3 per week. Multi-strain probiotics may be more effective than single-strain products, per a 2019 review in Advances in Nutrition. Results typically take two to four weeks to appear.
What is the fastest way to relieve severe constipation?
For immediate relief, a Fleet saline enema works within 1 to 5 minutes. A bisacodyl (Dulcolax) suppository works within 15 to 60 minutes. Oral stimulant laxatives like senna or bisacodyl tablets take 6 to 12 hours. High-dose magnesium citrate liquid (the 10 oz prep bottles) works within 30 minutes to 6 hours but should only be used occasionally due to electrolyte risks.
Can magnesium supplements cause diarrhea?
Yes, especially at higher doses. Magnesium draws water into the intestines, which is how it relieves constipation, but too much can cause loose stools or diarrhea. Start with 200 to 400 mg daily and increase gradually. Magnesium oxide is more likely to cause GI effects than magnesium glycinate (which is better absorbed). People with kidney disease should consult their doctor before taking magnesium supplements.
Is it safe to use enemas regularly for constipation?
No. Regular enema use (more than once per week) is not recommended. The Cleveland Clinic warns that frequent sodium phosphate enemas can cause dangerous electrolyte imbalances, including hyperphosphatemia, particularly in older adults and people with kidney problems. If you need enemas regularly, see a gastroenterologist to investigate the underlying cause.
What is the difference between a laxative and a stool softener?
Stool softeners (like docusate) only add moisture to stool to make it softer. Laxatives actively promote bowel movements through different mechanisms: osmotic laxatives (PEG, magnesium) draw water into the intestines, stimulant laxatives (senna, bisacodyl) trigger colon muscle contractions, and bulk-forming laxatives (psyllium) add fiber mass to stool. Most gastroenterologists consider osmotic laxatives more effective than traditional stool softeners for chronic constipation.

