If you’re over 50 and dealing with persistent bloating, sluggish digestion, or bowels that just won’t empty properly, you’re far from alone. A 2022 study published in Clinical Gastroenterology and Hepatology (the National GI Survey II, surveying 88,795 Americans) found that roughly 1 in 7 adults experience bloating weekly, and the rate climbs sharply after age 50. The good news: most bloating responds well to targeted dietary changes, specific supplements, and lifestyle shifts that support your gut microbiome from the inside out. According to gut microbiome research, this is supported by clinical evidence. According to bloating treatment guidelines, this is supported by clinical evidence.
I’ve spent years reviewing clinical evidence on digestive health, and what I keep coming back to is this: bloating is almost always a signal, not a standalone problem. It points to something deeper in your gut ecosystem that needs attention. In this guide, I’ll walk you through what causes bloating to worsen with age, which remedies for stomach bloating actually hold up under scrutiny, and how to build a long-term plan that keeps your digestion running smoothly.
Medical disclaimer: This article is for informational purposes only and does not replace professional medical advice. Always consult your healthcare provider before starting new supplements or making significant dietary changes, especially if you take prescription medications or have a diagnosed digestive condition.

Understanding Your Gut Microbiome After 50
Your gut houses roughly 100 trillion microorganisms, collectively called the gut microbiome. These bacteria, fungi, and other microbes do far more than digest food. They produce short-chain fatty acids (SCFAs) like butyrate, regulate immune responses, and even influence mood through the gut-brain axis. A 2021 study by Wilmanski et al., published in Nature Metabolism, linked microbiome diversity patterns directly to healthy aging and survival outcomes in older adults.
Here’s the problem: microbiome diversity naturally declines with age. Research from University College Cork, published in Nature (2012), showed that adults over 65 had measurably less diverse gut bacteria compared to younger adults. This decline correlates with increased inflammation, weaker immune function, and yes, more bloating and irregular bowel movements.
Your microbiome also shifts in composition. Beneficial bacteria like Bifidobacterium and certain Lactobacillus strains decrease, while potentially harmful species can gain ground. A 2021 review in Frontiers in Cellular and Infection Microbiology confirmed that this imbalance contributes to the digestive complaints so common in older adults.
Understanding this foundation matters because it changes how you approach treatment. Random supplements and generic advice won’t cut it. You need strategies that rebuild microbial diversity and support the specific functions your aging gut struggles with most.
Why Bloating Gets Worse After 50: The Real Causes
Bloating after 50 isn’t just about eating the wrong foods. Several age-related changes stack up to make your digestive system less efficient.
Reduced Stomach Acid Production
Your stomach produces less hydrochloric acid (HCl) as you age. A study published in the Journal of the American Geriatrics Society found that up to 30% of adults over 60 have atrophic gastritis, a condition where the stomach lining thins and acid output drops. Less acid means food sits in your stomach longer, ferments, and produces gas. It also means you absorb fewer nutrients from the food you eat, which can starve your beneficial gut bacteria.
Slower Gut Motility
The muscles in your digestive tract weaken with age, slowing the movement of food through your system. This is called decreased gut motility, and it’s a primary reason bowels stop emptying completely. The gut health supplement reviews we publish frequently address this issue because so many readers over 50 report the same frustration: feeling like things just aren’t moving.
Medication Side Effects
Many medications commonly prescribed to adults over 50, including proton pump inhibitors (PPIs), calcium channel blockers, opioid painkillers, and certain antidepressants, list bloating or constipation as side effects. Polypharmacy (taking five or more medications) is well-documented to increase the risk of gastrointestinal side effects, according to multiple clinical reviews. If you take multiple prescriptions, talk with your doctor about whether any could be contributing to your symptoms.
Hormonal Changes
For women, the drop in estrogen and progesterone during and after menopause directly affects gut motility and fluid retention. A 2020 study in Menopause (the journal of the North American Menopause Society) found that GI symptoms, including bloating and constipation, increased significantly during the menopausal transition. Men aren’t immune either: declining testosterone levels have been linked to changes in gut microbiome composition, with several studies showing correlations between androgen levels and microbial diversity.
Weakened Digestive Enzyme Production
Your pancreas produces fewer digestive enzymes over time, particularly lipase (for fats) and lactase (for dairy). This means foods you tolerated easily at 30 may now cause gas, cramping, and bloating at 55. The National Institute on Aging notes that lactose intolerance becomes increasingly common with age, affecting up to 68% of the global adult population.
Dietary Strategies That Actually Reduce Bloating
Before reaching for supplements, start with your plate. Dietary changes are the single most impactful thing you can do for gut health, and they cost nothing.
Get the Right Type of Fiber
Not all fiber is created equal, and getting this wrong is one of the most common mistakes I see. There are two main types:
- Soluble fiber dissolves in water, forms a gel, and feeds your beneficial gut bacteria. Sources include oats, barley, lentils, apples, and flaxseeds. This is the type that produces butyrate when fermented by your microbiome.
- Insoluble fiber adds bulk to stool and helps it move through your colon. Sources include whole wheat, vegetables, nuts, and seeds.
You need both, but the ratio matters. If you’re bloated and constipated, start by increasing soluble fiber gradually (add 2-3 grams per day over a week). Jumping straight to high-fiber cereals or massive salads often backfires, causing more gas and discomfort. A 2012 study in the World Journal of Gastroenterology found that a gradual increase in soluble fiber reduced bloating in 60% of participants with functional GI disorders.
Aim for 25-30 grams of total fiber daily. Most Americans get only about 15 grams, according to the USDA’s Dietary Guidelines for Americans (2020-2025).
Add Fermented Foods Strategically
Fermented foods like yogurt, kefir, sauerkraut, kimchi, and miso contain live bacteria that can temporarily boost your gut diversity. A landmark 2021 study from Stanford University, published in Cell, found that a diet high in fermented foods increased microbiome diversity and decreased markers of inflammation over 10 weeks.
Start small, though. One serving per day for the first week, then build to 2-3 servings. Some people experience temporary bloating when first introducing fermented foods as their microbiome adjusts.
Consider an Elimination Approach
If you suspect specific foods trigger your bloating, a structured elimination diet can help identify them. The low-FODMAP diet, developed at Monash University, has strong clinical evidence behind it. A 2016 meta-analysis in the European Journal of Nutrition found that the low-FODMAP approach reduced bloating symptoms in up to 75% of IBS patients.
Common trigger categories include:
- Dairy products (lactose)
- Wheat and rye (fructans)
- Onions and garlic (fructans)
- Beans and lentils (galacto-oligosaccharides)
- Certain fruits like apples, pears, and watermelon (excess fructose)
Work with a registered dietitian if possible. The elimination phase is temporary (2-6 weeks), followed by systematic reintroduction to identify your specific triggers.
Hydration and Meal Timing
Dehydration is an underrated cause of bloating and constipation. Water helps fiber do its job. Without enough of it, fiber can actually make constipation worse. Aim for at least 8 cups (64 ounces) daily, more if you exercise or take fiber supplements.
Meal timing matters too. Eating your largest meal at midday, when digestive enzyme production peaks, and keeping dinner lighter can reduce overnight bloating. Some clinical evidence suggests that time-restricted eating patterns may improve GI symptoms, though more research is needed in this area.
The Best Supplements for Gut Health, Bloating, and Regular Bowel Movements
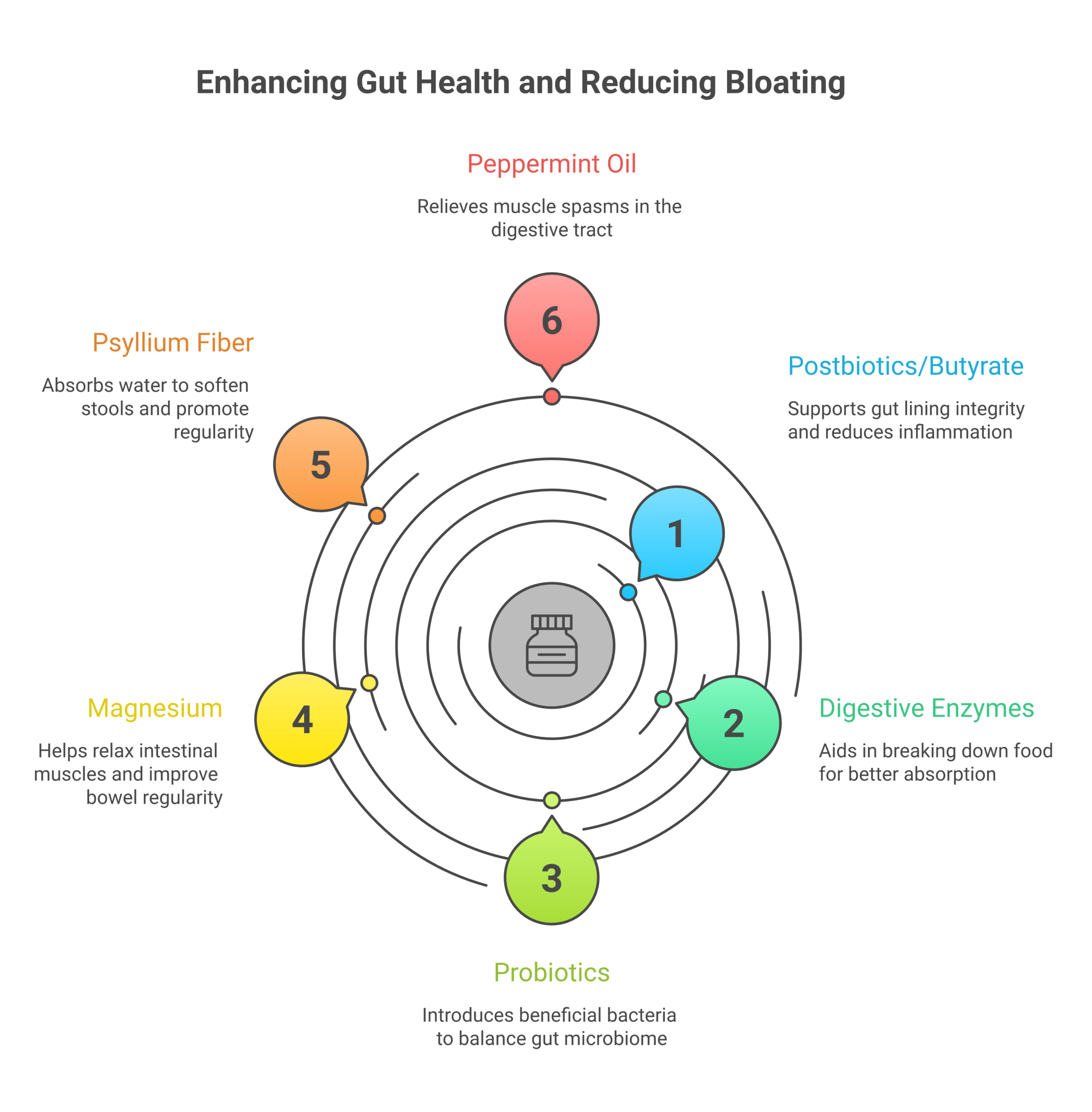
Once your diet is dialed in, the right biome supplements can accelerate your progress. Here’s what the evidence supports, ranked by strength of research.
Postbiotics and Butyrate: The Science-Backed Long-Term Solution
This is where the science gets really interesting, and where most people haven’t caught up yet. Postbiotics are bioactive compounds produced when beneficial bacteria ferment fiber in your gut. The most studied postbiotic is butyrate, a short-chain fatty acid that serves as the primary fuel source for the cells lining your colon.
Here’s why butyrate matters so much for bloating and bowel regularity:
- Strengthens the gut barrier: A 2024 review in the International Journal of Molecular Sciences confirmed that butyrate reinforces tight junctions between intestinal cells, reducing the “leaky gut” that contributes to inflammation and bloating.
- Reduces inflammation: Butyrate suppresses NF-kB, a key inflammatory pathway. A 2023 study in Gut Microbes showed that butyrate supplementation reduced markers of intestinal inflammation by up to 40% in animal models.
- Regulates motility: Butyrate stimulates the production of serotonin in the gut (where 95% of your body’s serotonin is made), which directly influences how quickly food moves through your digestive tract.
- Feeds beneficial bacteria: Butyrate creates a low-pH environment that favors the growth of beneficial species like Bifidobacterium and Faecalibacterium prausnitzii.
The challenge is that your body produces less butyrate as you age, precisely because the bacteria responsible for making it decline. This is why postbiotics and butyrate may outperform traditional probiotics for adults over 50. Instead of hoping that probiotic bacteria will survive stomach acid and colonize your gut, postbiotics deliver the end product directly.
The most bioavailable form of supplemental butyrate is tributyrin, a triglyceride that releases butyrate slowly throughout the intestinal tract. The patented form CoreBiome has been shown to deliver butyrate more efficiently than sodium butyrate or calcium butyrate in pharmacokinetic studies. You can read more about this in our detailed breakdown of why CoreBiome tributyrin is considered the gold standard.
If you’re looking for a postbiotic supplement, check our verified postbiotic supplement reviews for products we’ve independently tested.
Digestive Enzymes
If reduced enzyme production is contributing to your bloating (common after 50), a broad-spectrum digestive enzyme supplement can help. Look for formulas that include:
- Lipase (breaks down fats)
- Protease (breaks down proteins)
- Amylase (breaks down starches)
- Lactase (breaks down dairy sugars)
Johns Hopkins Medicine notes that digestive enzyme supplements can be particularly helpful for people with specific deficiencies, such as lactose intolerance or pancreatic insufficiency. Take them at the start of a meal for best results.
Probiotics: Choosing the Right Strains
Probiotics can help, but strain selection is critical. Not every probiotic addresses bloating. A 2019 meta-analysis in Alimentary Pharmacology and Therapeutics, covering 53 randomized controlled trials, found that specific strains reduced bloating significantly:
- Bifidobacterium infantis 35624: reduced bloating in IBS patients (Whorwell et al., 2006, American Journal of Gastroenterology)
- Lactobacillus plantarum 299v: improved bowel regularity and reduced gas (Ducrotté et al., 2012, World Journal of Gastroenterology)
- Saccharomyces boulardii: reduced antibiotic-associated bloating (McFarland, 2010, World Journal of Gastroenterology)
Multi-strain blends may also help. But here’s the honest truth: probiotics are a supporting player, not the star. The bacteria you swallow in a capsule are transient visitors. They pass through your system within days. For lasting change, you need to feed and support the bacteria already living in your gut, which is where postbiotics, fiber, and fermented foods come in.
Magnesium for Constipation and Bloating
Magnesium is one of the best supplements for regular bowel movements, and many adults over 50 don’t get enough. The National Institutes of Health estimates that 48% of Americans consume less than the recommended amount of magnesium from food alone.
Two forms work well for constipation:
- Magnesium citrate: draws water into the intestines (osmotic effect) and relaxes smooth muscle. A 2017 study in the European Journal of Clinical Nutrition found that magnesium citrate improved stool frequency and consistency in adults with functional constipation.
- Magnesium oxide: has a stronger laxative effect. Best for people with significant constipation, but can cause loose stools at higher doses.
Start with 200-400 mg of magnesium citrate daily and adjust based on results. If stools become too loose, reduce the dose.
Psyllium Husk Fiber
If you can’t get enough fiber from food alone, psyllium is the most studied supplemental fiber for bloating and constipation. A 2020 systematic review in the Journal of the American Association of Nurse Practitioners confirmed that psyllium improved stool consistency, frequency, and straining in patients with chronic constipation.
The key is starting low (one teaspoon per day) and drinking plenty of water with it. Build up to 2-3 teaspoons over 2-3 weeks. Taking too much too fast is the number one reason people give up on fiber supplements.
Lifestyle Changes That Support Gut Health
Supplements and diet get most of the attention, but lifestyle factors play a surprisingly large role in gut function.
Movement and Exercise
Regular physical activity stimulates gut motility. You don’t need intense workouts. A 2019 review in the Scandinavian Journal of Gastroenterology found that moderate exercise (brisk walking, cycling, swimming) for 30 minutes, 3-5 times per week, significantly improved constipation symptoms. Even a 10-15 minute walk after meals helps move gas through your system and reduces that post-meal bloating feeling.
Stress Management
Chronic stress directly impairs digestion through the gut-brain axis. Cortisol slows gut motility, alters microbiome composition, and increases intestinal permeability. Multiple clinical trials have found that 8-week mindfulness-based stress reduction programs improve IBS symptoms (including bloating) compared to standard care, with one randomized trial reporting a 71% responder rate for GI symptom improvement.
Practical options include deep breathing exercises before meals, regular meditation (even 10 minutes daily), adequate sleep (7-8 hours), and limiting late-night screen time, which disrupts circadian rhythms tied to gut function.
Eating Habits
How you eat matters as much as what you eat:
- Chew thoroughly (20-30 chews per bite reduces air swallowing and improves mechanical digestion)
- Eat without screens or distractions
- Don’t drink large amounts of liquid during meals (small sips are fine)
- Avoid carbonated beverages, which introduce CO2 directly into your GI tract
- Don’t lie down within 2-3 hours of eating
Managing Diverticulosis and Bloating
Diverticulosis, the formation of small pouches in the colon wall, affects roughly 58% of adults over 60 according to a 2018 review in Gastroenterology Clinics of North America. These pouches can trap food and bacteria, contributing to chronic bloating, irregular bowel movements, and abdominal discomfort.
If you’ve been diagnosed with diverticulosis, here’s what the current evidence supports for supplements for diverticulosis management:
Fiber Is Still the Foundation
The American Gastroenterological Association (AGA) recommends a fiber-rich diet for patients with diverticulosis. A high-fiber diet softens stool, reduces colon pressure, and may slow the progression of new diverticula. Psyllium is particularly useful here because it regulates stool consistency without causing the excess gas that wheat bran sometimes does.
Old advice to avoid seeds, nuts, and popcorn has been debunked. A large 2008 study in JAMA involving 47,228 men found no increased risk of diverticulitis from consuming nuts, corn, or popcorn. The AGA no longer recommends these restrictions.
Butyrate for Colon Health
Butyrate is especially relevant for people with diverticulosis. Since it serves as the primary energy source for colonocytes (the cells lining your colon), adequate butyrate levels support tissue repair and reduce inflammation in the areas most affected by diverticula. A 2022 study in Nutrients suggested that butyrate-producing bacteria were significantly reduced in patients with symptomatic diverticular disease compared to healthy controls.
This makes a strong case for combining a high-fiber diet (to feed butyrate-producing bacteria) with tributyrin supplementation (to deliver butyrate directly). Our guide on what to look for in a superior postbiotic supplement covers the specific quality markers to prioritize.
Probiotics for Diverticulosis
A 2016 review in Therapeutic Advances in Gastroenterology found that certain probiotic strains (Lactobacillus casei and Lactobacillus acidophilus) reduced symptoms in patients with uncomplicated diverticular disease. The evidence is moderate, not definitive, but worth considering as part of a broader strategy.
Building Your Daily Gut Health Routine
Here’s a practical daily framework that pulls together everything above:
Morning:
- Glass of warm water with lemon (stimulates digestive secretions)
- Fiber-rich breakfast (oatmeal with ground flaxseed, or whole-grain toast with avocado)
- Postbiotic/tributyrin supplement with breakfast
- Magnesium citrate (200 mg) if constipation is a concern
Midday:
- Largest meal of the day (when enzyme production peaks)
- Digestive enzyme supplement if needed (take at start of meal)
- One serving of fermented food (yogurt, kimchi, or sauerkraut)
Afternoon:
- 10-15 minute walk
- Second serving of fermented food or a probiotic supplement
Evening:
- Lighter dinner, eaten at least 3 hours before bed
- Herbal tea (peppermint or ginger, both supported by evidence for reducing gas and bloating)
- Psyllium husk with a full glass of water (if supplementing fiber)
Adjust this framework based on what works for your body. Track your symptoms for 2-3 weeks when making changes so you can identify what actually helps versus what doesn’t.
When to See a Doctor
Most bloating responds to the dietary, supplement, and lifestyle strategies outlined here. But certain symptoms warrant prompt medical attention:
- Blood in your stool (bright red or dark/tarry)
- Unintentional weight loss of more than 5% of body weight over 6-12 months
- Persistent pain that doesn’t resolve with passing gas or a bowel movement
- New onset of symptoms after age 50 with no prior history of GI issues
- Difficulty swallowing or a feeling of food getting stuck
- Fever or vomiting accompanying bloating episodes
- Family history of colorectal cancer, inflammatory bowel disease, or celiac disease
These could indicate conditions that need diagnostic workup, including colonoscopy, imaging, or blood tests. The American Cancer Society recommends that all adults begin regular colorectal cancer screening at age 45.
If you’ve already seen a doctor and been cleared of serious conditions, the strategies in this guide give you a strong, evidence-based foundation for long-term gut health improvement.
The Bottom Line
Bloating and irregular bowel movements after 50 are common, but they’re not inevitable. The research points clearly toward a multi-pronged approach: rebuild your gut microbiome through fiber and fermented foods, address specific deficiencies with targeted supplements, and support digestion through daily movement and stress management.
Among the supplement options available, postbiotics, specifically butyrate in the tributyrin form, stand out as the most promising long-term solution. They address the root cause (declining SCFA production) rather than just managing symptoms. Combined with the right fiber intake, adequate magnesium, and appropriate probiotic strains, most people see meaningful improvement within 4-8 weeks.
Ready to find a quality postbiotic supplement? Browse our verified postbiotic supplement reviews, where every product has been independently evaluated for ingredient quality, dosage, and clinical evidence.
For more evidence-based guidance, explore our Consumer Health Guide homepage or learn more about our review methodology.
You may also want to read our guide on vitamins for eye health.
Frequently Asked Questions
What are the best remedies for stomach bloating after age 50?
The most effective approach combines dietary changes (increased soluble fiber, fermented foods, elimination of trigger foods) with targeted supplements. Postbiotics like tributyrin-based butyrate, digestive enzymes, strain-specific probiotics, and magnesium citrate all have clinical support. Start with diet first, then add supplements based on your specific symptoms.
Why do my bowels feel like they’re not emptying completely?
Incomplete evacuation is often caused by reduced gut motility, insufficient fiber intake, dehydration, or pelvic floor dysfunction. Medications like PPIs, calcium channel blockers, and opioids can also contribute. Increasing fiber gradually, staying well-hydrated, regular exercise, and magnesium supplementation typically improve this symptom. If it persists, consult a gastroenterologist to rule out pelvic floor issues or other conditions.
Are postbiotics better than probiotics for gut health?
For many adults over 50, yes. Probiotics deliver live bacteria that must survive stomach acid, compete with existing microbes, and successfully colonize your gut, which is a tall order. Postbiotics like butyrate skip that process entirely and deliver the beneficial end product directly. A 2025 review in Frontiers in Microbiomes found that postbiotics offered comparable or superior outcomes to probiotics for gut barrier function and inflammation.
What supplements help with diverticulosis symptoms?
Psyllium fiber is the first-line supplement, as it softens stool and reduces colon pressure. Butyrate (tributyrin form) supports colonocyte health and reduces local inflammation. Certain probiotic strains like Lactobacillus casei have shown moderate benefit. Magnesium citrate can help if constipation is a primary symptom. Always increase fiber gradually and with adequate water intake.
How long does it take for gut health supplements to work?
Most people notice initial improvements within 1-2 weeks, particularly with magnesium and digestive enzymes. Probiotics typically need 2-4 weeks to show effects. Postbiotics and fiber supplements generally produce noticeable changes in bloating and regularity within 2-4 weeks, with continued improvement over 8-12 weeks as your microbiome adapts. Consistency matters more than any single product.
Can I take multiple gut health supplements at the same time?
Yes, and in many cases combining supplements produces better outcomes than any single product alone. A reasonable stack for someone over 50 with bloating and constipation might include a tributyrin-based postbiotic, magnesium citrate, and psyllium fiber. Space them out if needed (postbiotic with breakfast, magnesium at bedtime, fiber in the evening). Always check with your healthcare provider about interactions with prescription medications.
What’s the best for constipation and bloating at the same time?
Magnesium citrate addresses both issues simultaneously by drawing water into the colon (softening stool) and relaxing smooth muscle (reducing cramping and gas retention). Psyllium fiber also helps both by normalizing stool consistency and feeding butyrate-producing bacteria. For long-term improvement, adding a tributyrin-based postbiotic supplement supports the gut lining and promotes healthy motility. Start with magnesium and fiber, then layer in a postbiotic for best results.