Medical Disclaimer: This content is for informational purposes only and does not replace professional medical advice. Consult your healthcare provider before starting any supplement regimen.
Constipation is one of the most common digestive complaints worldwide, affecting roughly 16% of all adults and up to 33% of adults over age 60, according to the National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK). If you are dealing with infrequent bowel movements, hard stools, or the uncomfortable feeling that you cannot fully empty your bowels, you are not alone. The good news: most cases of constipation respond well to dietary changes, lifestyle adjustments, and targeted supplements. In this guide from Consumer Health Guide, we break down constipation causes and treatment options so you can take clear, informed action.
What Is Constipation?
Doctors generally define constipation as having fewer than three bowel movements per week, though individual patterns vary. The Rome IV diagnostic criteria, published by the Rome Foundation in 2016, also include symptoms like straining during more than 25% of bowel movements, lumpy or hard stools, a sensation of incomplete evacuation, and the need for manual maneuvers to pass stool. Chronic constipation means these symptoms persist for at least three months.
Constipation is not a disease on its own. It is a symptom that can point to dietary gaps, medication side effects, or underlying medical conditions. Understanding what drives your symptoms is the first step toward effective relief.
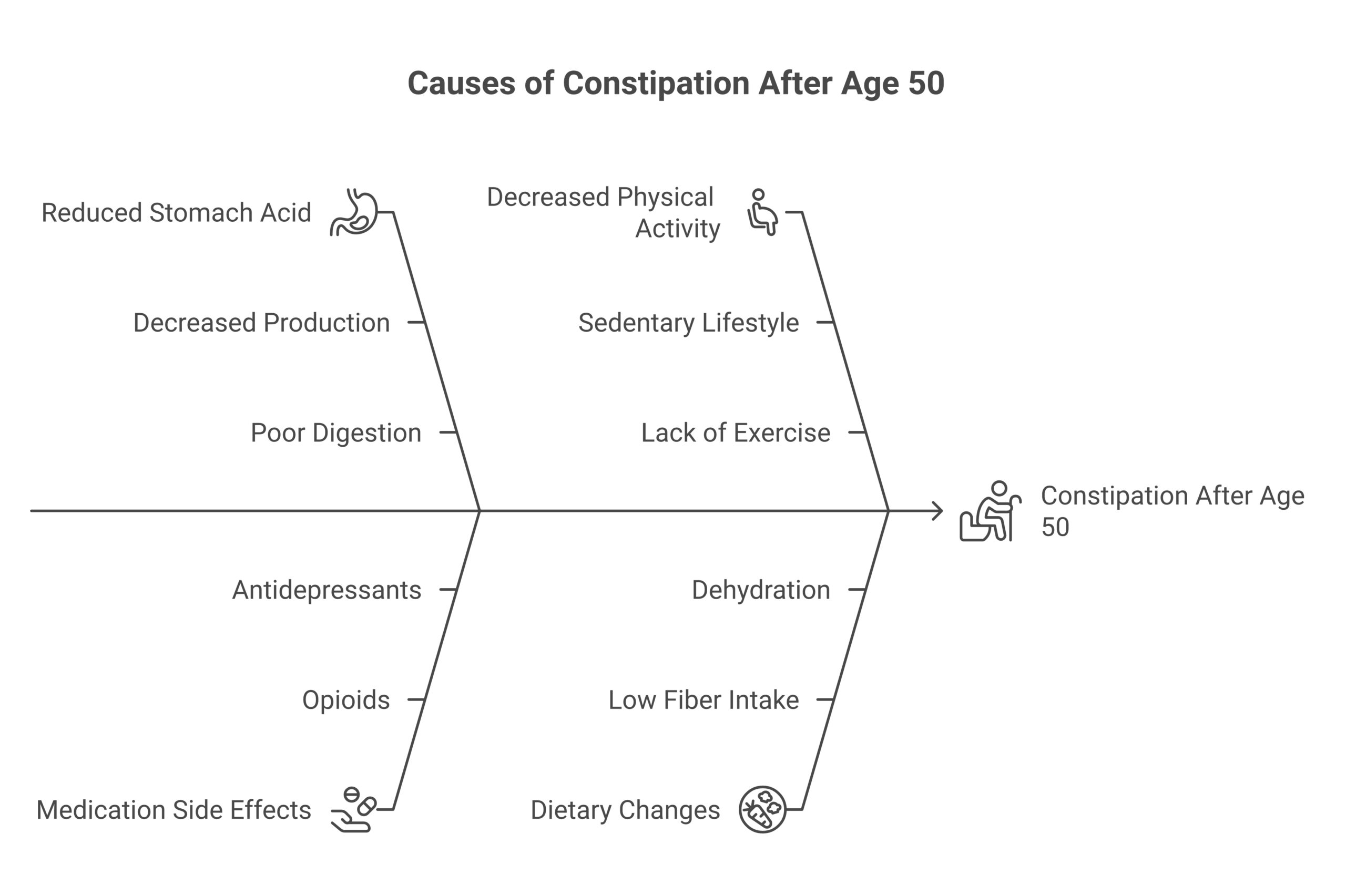
Common Causes of Constipation
Constipation rarely has a single cause. More often, several factors combine to slow your digestive system. Below are the most frequent contributors.
Dietary Factors
A low-fiber diet is the number one dietary cause. The American Society of Colon and Rectal Surgeons recommends 25 to 31 grams of fiber daily for adults, yet USDA data from its 2020 Dietary Guidelines for Americans shows the average American eats only about 15 grams per day. Without enough fiber, stool loses bulk and moves slowly through the colon.
Dehydration compounds the problem. When your body lacks water, the colon absorbs more fluid from stool, leaving it dry and hard. The NIDDK lists inadequate fluid intake as a contributing factor to constipation, and multiple clinical reviews have found that increasing water intake can improve stool consistency in people who are under-hydrated.
Processed foods, dairy-heavy diets, and excessive alcohol consumption also slow transit time. If you want to learn how diet and gut health connect, read our guide on the best foods for gut health.
Medications That Cause Constipation
Certain prescription and over-the-counter drugs are well-known culprits:
- Opioid pain medications (oxycodone, hydrocodone, morphine): The American Gastroenterological Association (AGA) estimates that 40% to 80% of patients taking opioids develop opioid-induced constipation.
- Iron supplements: A 2020 review in Nutrients confirmed that ferrous sulfate, the most commonly prescribed form of iron, frequently causes constipation and other GI side effects.
- Calcium channel blockers (amlodipine, diltiazem): These blood pressure medications relax smooth muscle in the colon, slowing motility.
- Anticholinergic drugs (certain antihistamines, antidepressants, bladder medications): They reduce gut contractions.
- GLP-1 receptor agonists (semaglutide, tirzepatide): These newer weight-loss and diabetes medications delay gastric emptying. A 2023 cohort study by Sodhi et al. in JAMA found that GLP-1 receptor agonist users had significantly higher risks of gastroparesis (hazard ratio 3.67), bowel obstruction (hazard ratio 4.22), and pancreatitis (hazard ratio 9.09) compared to users of other weight-loss medications. Constipation is also a commonly reported side effect in clinical trials of these drugs.
- Antacids containing aluminum or calcium
If you suspect a medication is contributing to your constipation, talk to your prescribing physician before making any changes.
Lifestyle and Behavioral Factors
Sedentary habits matter more than most people realize. The NIDDK identifies physical inactivity as a major risk factor for constipation. Exercise stimulates peristalsis, the wave-like muscle contractions that push food through the digestive tract.
Ignoring the urge to go is another common trigger. When you repeatedly suppress the defecation reflex, the rectum becomes less sensitive over time, and stool hardens as water continues to be absorbed.
Travel, disrupted routines, and stress can also slow things down. The enteric nervous system (sometimes called the “second brain”) responds to emotional states, and research on the gut-brain axis has consistently linked perceived stress to increased self-reported constipation.
Medical Conditions
Several health conditions list constipation as a primary symptom:
| Condition | Why It Causes Constipation |
|---|---|
| Hypothyroidism | Low thyroid hormones slow metabolism and gut motility |
| Diabetes (Type 1 and Type 2) | Nerve damage (diabetic neuropathy) can impair colon function |
| Irritable Bowel Syndrome (IBS-C) | Disordered gut-brain signaling causes chronic constipation with pain |
| Parkinson’s Disease | Neurodegeneration affects the enteric nervous system years before motor symptoms |
| Multiple Sclerosis | Nerve damage disrupts signals between brain and bowel |
| Pelvic floor dysfunction | Muscles that coordinate defecation fail to relax properly |
| Colorectal strictures or tumors | Physical blockage prevents stool passage |
If your constipation is persistent and does not respond to dietary changes, your doctor may test for these conditions.
The Gut Microbiome Connection
A February 2026 study from Nagoya University, published in Gut Microbes, identified two gut bacteria, Akkermansia muciniphila and Bacteroides thetaiotaomicron, that work together to degrade the protective mucus lining of the colon. When this mucus layer thins, stool dries out and becomes harder to pass. The researchers noted this mechanism helps explain why traditional laxatives fail for many people with chronic constipation. The gut microbiome is increasingly recognized as a factor in bowel regularity, and supporting microbial balance through diet and targeted supplementation may offer a path forward. Our article on postbiotics vs probiotics covers these newer approaches in detail.
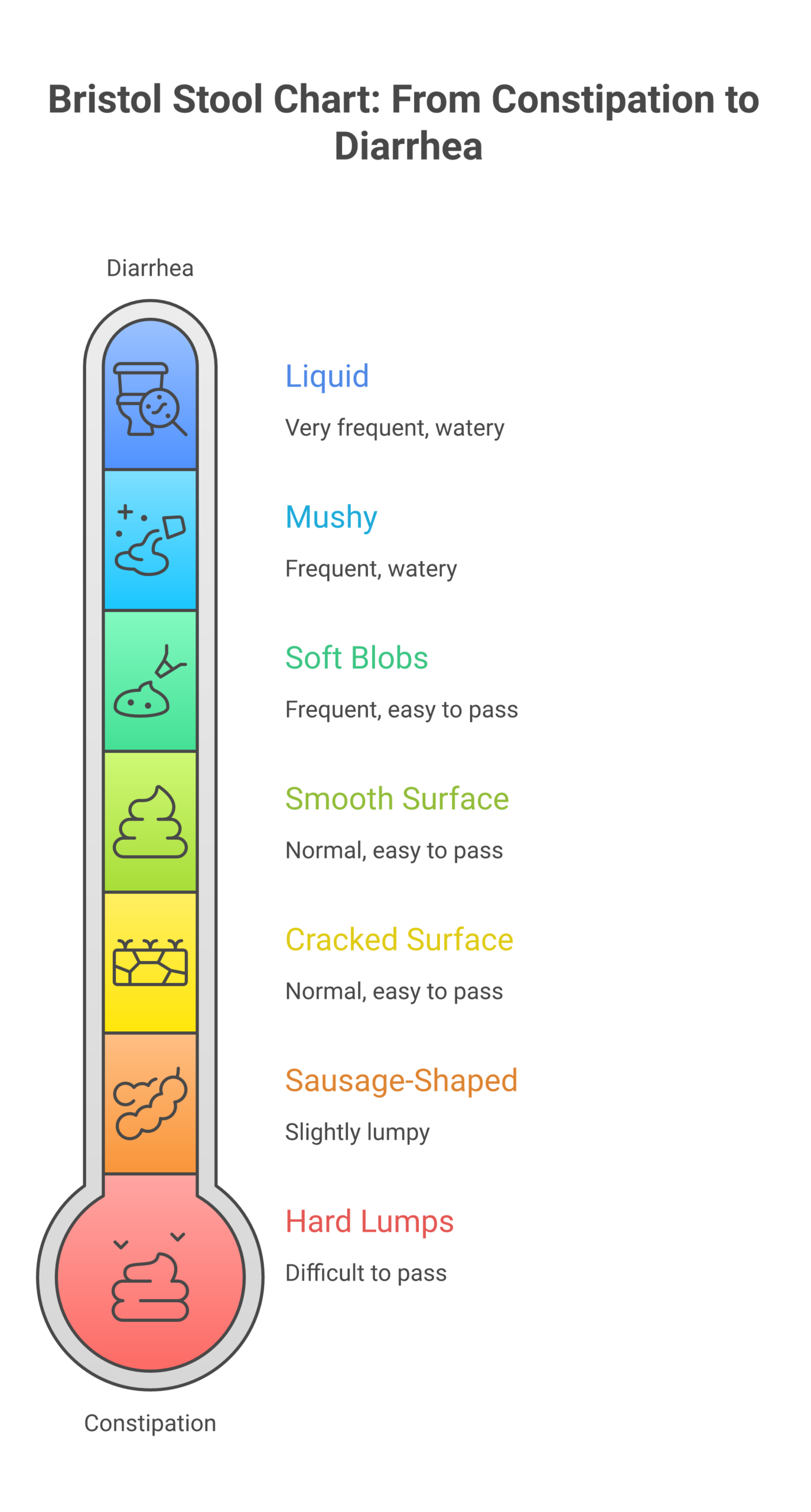
Symptoms of Constipation and Warning Signs
Typical constipation symptoms include:
- Fewer than three bowel movements per week
- Hard, dry, or lumpy stools
- Straining or pain during bowel movements
- Feeling of incomplete evacuation
- Abdominal bloating or discomfort
- Needing to press on your abdomen or use a finger to help pass stool
When to See a Doctor
Most constipation is temporary and responds to self-care. However, the Mayo Clinic advises seeking medical attention if you experience:
- Constipation lasting more than three weeks despite home remedies
- Blood in your stool or on the toilet paper
- Unexplained weight loss
- Severe abdominal pain
- A sudden, unexplained change in bowel habits after age 50
- Thin, pencil-like stools (which may indicate a structural issue)
These symptoms can signal conditions that require prompt evaluation, including colorectal cancer.
Natural Ways to Treat Constipation
Before reaching for medication, try these evidence-based lifestyle and dietary strategies. They address root causes rather than just symptoms.
Increase Dietary Fiber Gradually
A 2016 systematic review by Christodoulides et al. in Alimentary Pharmacology & Therapeutics found that 77% of patients with chronic constipation improved with fiber supplementation compared to 44% on placebo. The key word is “gradually.” Adding too much fiber too fast causes gas and bloating.
Target 25 to 30 grams per day from a mix of soluble and insoluble sources:
- Soluble fiber (absorbs water, softens stool): oats, beans, lentils, apples, citrus fruits, psyllium husk
- Insoluble fiber (adds bulk, speeds transit): whole wheat, bran, vegetables, nuts
Psyllium husk stands out in clinical research. The Canadian Association of Gastroenterology identifies psyllium as the most studied bulking agent, shown to decrease stool transit time and improve both frequency and consistency. Our gut health supplement reviews cover fiber supplements in more depth.
Drink More Water
Fiber needs water to work. Without adequate hydration, high-fiber diets can actually worsen constipation. The National Academies of Sciences, Engineering, and Medicine (2004) recommend about 3.7 liters of total daily fluid for men and 2.7 liters for women, including fluids from food. Plain water is best. Caffeinated beverages offer mild stimulant effects on the colon but can be dehydrating in large amounts.
Move Your Body
Regular physical activity is one of the most effective natural ways to treat constipation. A 2019 systematic review and meta-analysis in the Scandinavian Journal of Gastroenterology (Gao et al.) found that aerobic exercise, including brisk walking, significantly improved constipation symptoms across nine randomized controlled trials.
You do not need to run marathons. Walking, cycling, swimming, and yoga all stimulate gut motility. Even 15 to 20 minutes of daily movement can make a measurable difference.
Establish a Bowel Routine
The NIDDK recommends trying to have a bowel movement at the same time each day, ideally 15 to 45 minutes after breakfast. The gastrocolic reflex, a natural increase in colon activity triggered by eating, is strongest in the morning. Sitting on the toilet for 5 to 10 minutes at this time (without straining) can retrain your body’s rhythm.
A squatting position, or using a footstool to elevate your knees above your hips, can relax the puborectalis muscle and straighten the anorectal angle. A 2019 study in the Journal of Clinical Gastroenterology found that a toilet footstool reduced bowel movement duration in 71% of participants, with 90% reporting less straining.
Manage Stress
Chronic stress affects gut motility through the gut-brain axis. Cognitive behavioral therapy (CBT), meditation, and deep breathing exercises have all shown benefits for functional constipation in clinical trials. The American College of Gastroenterology recommends gut-directed CBT as an effective behavioral therapy for IBS-C, with multiple trials showing meaningful reductions in constipation severity.
Over-the-Counter Treatment Options
When lifestyle changes alone are not enough, several OTC products can help. Here is what the evidence says about each type.
Bulk-Forming Laxatives
Products like Metamucil (psyllium), Citrucel (methylcellulose), and FiberCon (calcium polycarbophil) add fiber to your stool. They are considered the safest long-term option by the American College of Gastroenterology (ACG). Take them with plenty of water.
Osmotic Laxatives
These draw water into the colon to soften stool. Common options include:
- Polyethylene glycol (MiraLAX): The ACG’s 2021 clinical guideline rates polyethylene glycol as a first-line treatment with strong evidence supporting its effectiveness.
- Magnesium citrate: Works quickly (usually within 30 minutes to 6 hours) but is best for occasional use.
- Lactulose: A prescription osmotic that also has prebiotic effects, feeding beneficial gut bacteria.
Stool Softeners
Docusate sodium (Colace) pulls water and fat into stool. It is gentle and often recommended for post-surgical patients. However, a 2010 Cochrane review found limited evidence for docusate’s effectiveness compared to psyllium, and the ACG notes that it may be less effective than osmotic laxatives for chronic constipation.
Stimulant Laxatives
Bisacodyl (Dulcolax) and senna (Senokot) stimulate nerve endings in the colon to increase muscle contractions. They work within 6 to 12 hours. While older guidelines warned against long-term use, a 2020 position paper from the AGA clarified that stimulant laxatives are safe for chronic use when needed and do not cause colon damage or dependence when used at recommended doses.
Lubricant Laxatives
Mineral oil coats stool with a waterproof film, preventing moisture loss. It is effective but not recommended for long-term use because it can interfere with absorption of fat-soluble vitamins (A, D, E, K).
Supplements That Support Bowel Regularity
Beyond standard OTC laxatives, certain supplements have clinical evidence behind them for constipation relief.
Magnesium
Magnesium oxide, citrate, and hydroxide all have osmotic properties that draw water into the intestines. A 2021 study in Nutrients found that magnesium supplementation significantly improved stool frequency and consistency in adults with mild to moderate constipation. Magnesium also supports muscle relaxation throughout the GI tract.
Probiotics
A 2014 meta-analysis in the American Journal of Clinical Nutrition reviewed 14 randomized controlled trials and found that probiotics increased weekly bowel movements by an average of 1.3 per week. Bifidobacterium lactis was the most consistently effective strain. Probiotics work by modulating gut flora, producing short-chain fatty acids, and improving colonic motility.
Postbiotics and Butyrate
Postbiotics are bioactive compounds produced by probiotic bacteria during fermentation. Butyrate, a short-chain fatty acid, plays a direct role in colon health. It fuels colonocytes (the cells lining the colon), strengthens the intestinal barrier, and regulates motility. Early clinical research, including a 2014 trial published in Przegląd Gastroenterologiczny (Banasiewicz et al.), found that sodium butyrate supplementation reduced the percentage of patients reporting constipation and improved stool consistency.
Tributyrin, a triglyceride form of butyrate, survives stomach acid better than sodium butyrate. CoreBiome is a patented tributyrin ingredient with published bioavailability data. For a closer look at this category, see our guide on tributyrin and CoreBiome.
Choosing the right gut health supplement can feel overwhelming. Our team has reviewed dozens of products. Check our verified gut health supplement reviews to find options backed by third-party testing and clinical evidence.
Fiber Supplements
If you struggle to get enough fiber from food alone, supplements can fill the gap. Psyllium husk (Metamucil) has the strongest evidence base, but partially hydrolyzed guar gum (PHGG) is another well-studied option. A 2012 trial in Nutrition found that 5 grams of PHGG daily improved bowel frequency in adults with chronic constipation without causing the bloating that some people experience with psyllium.
Prescription Medications for Chronic Constipation
When OTC options and supplements are not sufficient, doctors can prescribe targeted medications. These are typically reserved for chronic idiopathic constipation (CIC) or IBS-C that has not responded to first-line treatments.
Secretagogues
- Lubiprostone (Amitiza): A chloride channel activator that increases intestinal fluid secretion. FDA-approved for CIC and IBS-C. Pivotal trials showed it significantly increased spontaneous bowel movements compared to placebo, leading to FDA approval for CIC and IBS-C.
- Linaclotide (Linzess): A guanylate cyclase-C agonist that increases intestinal fluid and reduces visceral pain. Particularly useful for IBS-C patients who experience abdominal discomfort along with constipation.
- Plecanatide (Trulance): Similar mechanism to linaclotide, FDA-approved for CIC and IBS-C.
Prokinetic Agents
- Prucalopride (Motegrity): A selective serotonin 5-HT4 receptor agonist that stimulates colonic motility. A 2019 review in Drugs confirmed its effectiveness for chronic constipation with a favorable safety profile.
Opioid-Induced Constipation Treatments
- Naloxegol (Movantik) and methylnaltrexone (Relistor): These peripherally acting mu-opioid receptor antagonists (PAMORAs) block opioid effects in the gut without affecting pain relief. The AGA recommends them as first-line pharmacotherapy for opioid-induced constipation that has not responded to laxatives.
Medical Procedures for Severe Constipation
In rare cases where medications and behavioral therapies fail, doctors may consider procedural interventions.
Biofeedback Therapy
For patients with pelvic floor dysfunction (dyssynergic defecation), biofeedback is the treatment of choice. It uses sensors and visual feedback to retrain the muscles involved in defecation. A randomized controlled trial by Heymen et al., published in Diseases of the Colon & Rectum (2007), found that 70% of patients receiving biofeedback reported adequate relief compared to 23% with diazepam.
Sacral Nerve Stimulation
This therapy delivers mild electrical pulses to the sacral nerves that control bowel function. Originally developed for urinary incontinence, it has shown promise for chronic constipation in patients who do not respond to other treatments. Clinical trials have shown improvement in a subset of patients treated with sacral nerve stimulation, though response rates vary and patient selection is important.
Surgery
Surgical options are a last resort. A subtotal colectomy (removal of most of the colon) may be considered for patients with severe slow-transit constipation who have failed all medical therapies. The Cleveland Clinic reports that outcomes vary, with up to 90% of carefully selected patients experiencing improvement. However, the procedure carries risks including diarrhea, incontinence, and abdominal pain.
Constipation in Special Populations
Pregnancy
Constipation affects an estimated 25% to 40% of pregnant women, according to the American College of Obstetricians and Gynecologists (ACOG). Rising progesterone levels relax smooth muscle throughout the body, including the colon. Iron supplements prescribed during pregnancy add to the problem. ACOG recommends fiber, fluids, and physical activity as first-line approaches. Bulk-forming laxatives like psyllium are generally considered safe. Stimulant laxatives should be used with caution and only under a provider’s guidance.
Older Adults
Constipation prevalence rises sharply after age 65. Contributing factors include reduced physical activity, polypharmacy (multiple medications), decreased fluid intake, and weakened pelvic floor muscles. The AGS Beers Criteria (2023 update) cautions against regular use of certain laxatives in older adults and recommends starting with fiber and osmotic agents.
Children
Functional constipation is common in children, with a 2018 meta-analysis in the Journal of Pediatrics (Koppen et al.) estimating a pooled worldwide prevalence of about 9.5%, though individual studies reported rates ranging from 0.5% to 32%. Withholding behavior after a painful bowel movement is a common trigger. The North American Society for Pediatric Gastroenterology, Hepatology, and Nutrition (NASPGHAN) recommends polyethylene glycol as first-line treatment for children, combined with behavioral interventions and dietary changes.
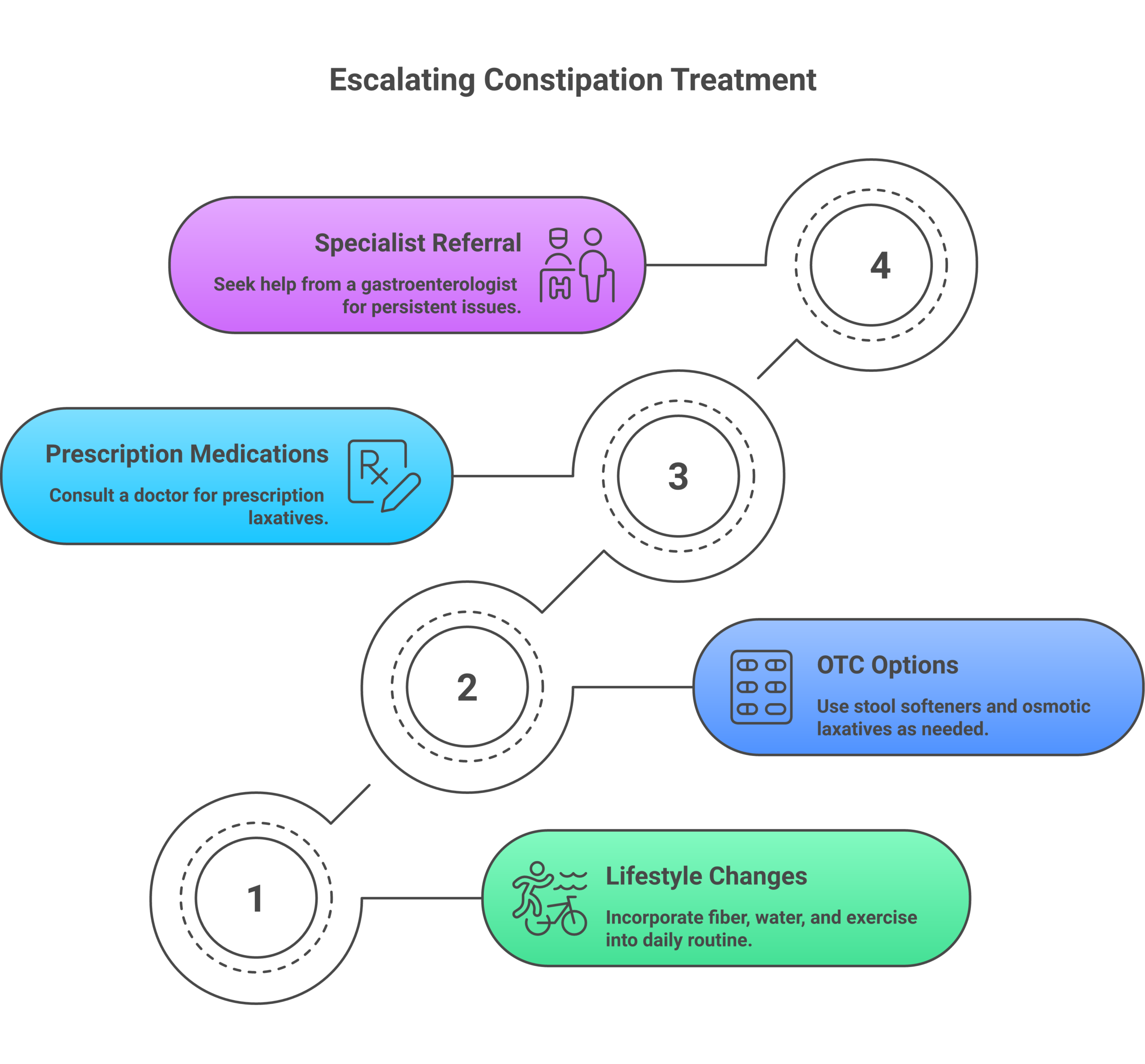
How to Build a Complete Constipation Relief Plan
Constipation rarely has a single fix. The most effective approach combines several strategies tailored to your specific situation.
Start here:
- Increase fiber to 25 to 30 grams per day (gradually, over 2 weeks)
- Drink at least 8 cups of water daily
- Walk or exercise for at least 20 to 30 minutes most days
- Set a consistent morning toilet time, 15 to 45 minutes after breakfast
- Review your medications with your doctor for constipation-causing drugs
If those steps are not enough after 2 to 3 weeks:
- Try a bulk-forming or osmotic laxative (psyllium or MiraLAX)
- Consider a magnesium supplement (200 to 400 mg daily)
- Add a probiotic with Bifidobacterium strains
- Look into postbiotic or butyrate supplementation for gut barrier support
If constipation persists beyond 6 weeks:
- See a gastroenterologist for evaluation
- Ask about prescription options (linaclotide, prucalopride)
- Consider biofeedback if pelvic floor dysfunction is suspected
Understanding what to look for in supplements matters. Our postbiotic supplement guide walks through ingredient quality, dosing, and what the research actually supports.
You may also want to read our guide on eye health supplements.
Frequently Asked Questions About Constipation
What is the most common cause of constipation?
Low dietary fiber intake is the most frequently cited cause. The USDA reports that the average American adult consumes only about 15 grams of fiber per day, well below the recommended 25 to 31 grams. Inadequate water intake and a sedentary lifestyle compound the problem. Addressing these three factors resolves constipation for most people.
How long is too long to be constipated?
If you have not had a bowel movement for more than three days, or if constipation persists for more than three weeks despite dietary changes, the Mayo Clinic recommends seeing a doctor. Seek immediate attention if you experience severe abdominal pain, vomiting, or blood in your stool.
Are laxatives safe to take every day?
Bulk-forming laxatives (psyllium, methylcellulose) and osmotic laxatives (polyethylene glycol) are generally safe for daily, long-term use according to the American College of Gastroenterology. Stimulant laxatives (bisacodyl, senna) were once thought to cause dependence, but a 2020 AGA position paper confirmed they are safe for chronic use at recommended doses. That said, long-term laxative use should be monitored by your healthcare provider.
Can constipation cause other health problems?
Yes. Chronic constipation can lead to hemorrhoids from straining, anal fissures (small tears in the anus), fecal impaction (hardened stool stuck in the rectum), and rectal prolapse in severe cases. A 2018 study in Clinical Gastroenterology and Hepatology also linked chronic constipation to an increased risk of cardiovascular events, possibly through shared mechanisms involving gut microbiome disruption and systemic inflammation.
Do probiotics help with constipation?
Yes, for many people. A 2014 meta-analysis of 14 randomized controlled trials published in the American Journal of Clinical Nutrition found that probiotics increased bowel movement frequency by an average of 1.3 times per week. Bifidobacterium lactis showed the most consistent results. Probiotics are not a quick fix, though. Most studies saw benefits after 2 to 4 weeks of daily use.
What foods should I avoid if I am constipated?
Reduce or temporarily eliminate processed foods, red meat, dairy products (especially cheese), fried foods, and white bread or pasta. Alcohol and excessive caffeine can also contribute to dehydration and worsen symptoms. Focus instead on whole grains, fruits, vegetables, legumes, and adequate water intake.
Is chronic constipation a sign of something serious?
In most cases, chronic constipation results from dietary and lifestyle factors. However, it can sometimes indicate conditions like hypothyroidism, diabetes, pelvic floor dysfunction, or colorectal cancer. The American Cancer Society recommends that adults at average risk begin colorectal cancer screening at age 45. If your constipation is new, persistent, or accompanied by weight loss, blood in stool, or severe pain, see your doctor promptly.
Still researching what helps relieve constipation from the supplement side? Browse our verified gut health supplement reviews for evidence-based product comparisons reviewed by our review methodology team.