The best natural cough remedies include honey, thyme tea, marshmallow root, ginger, saltwater gargles, and steam inhalation. For stubborn coughs, over-the-counter options like dextromethorphan (a cough suppressant) and guaifenesin (an expectorant) can help. A 2021 systematic review published in BMJ Evidence-Based Medicine found that honey outperformed standard care for reducing cough frequency and severity in upper respiratory infections. Below, we break down each option with the clinical evidence behind it so you can choose the best medicine for a bad cough based on your symptoms.
What Causes a Cough
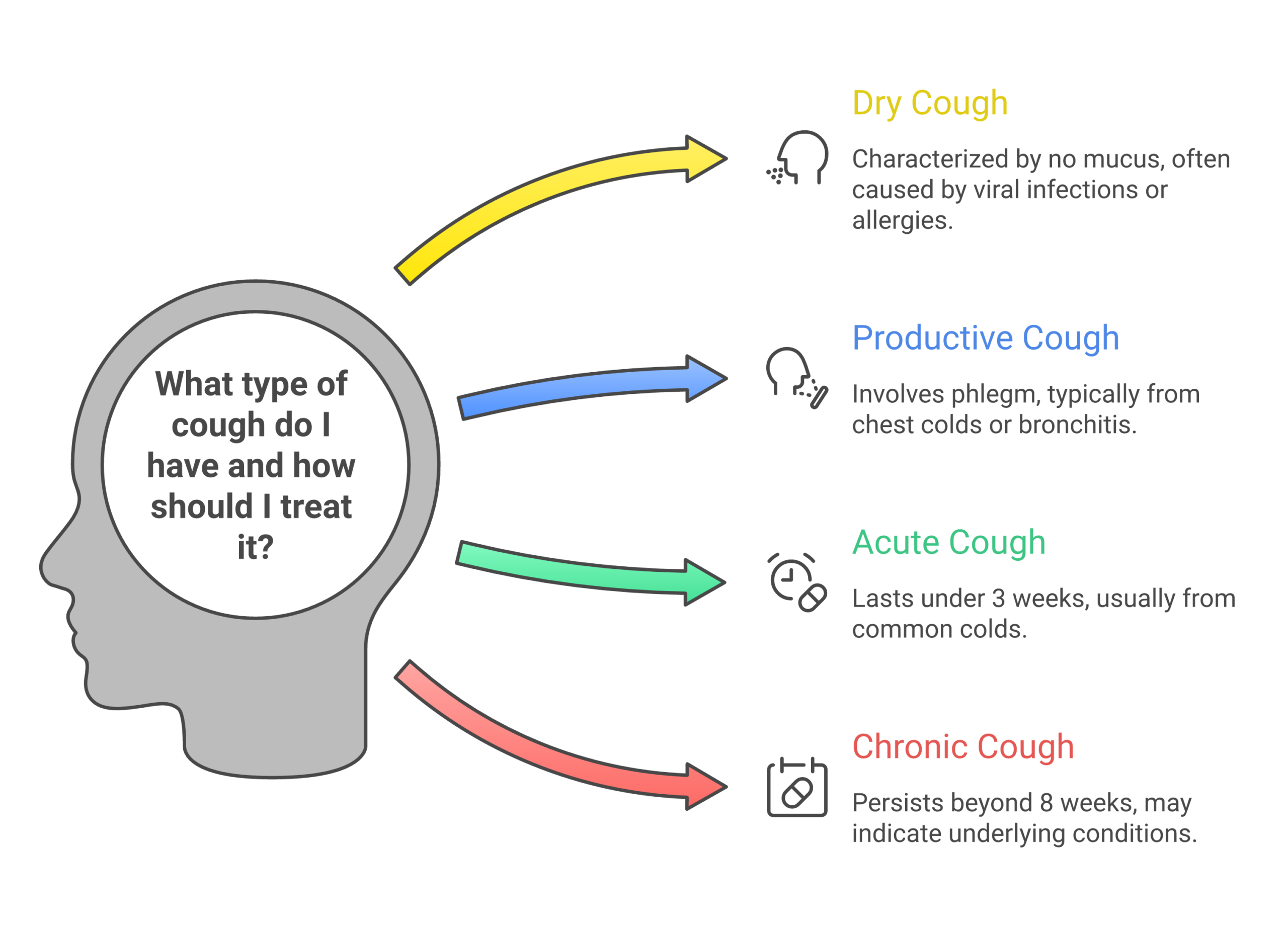
A cough is your body’s reflex for clearing irritants from your airways. It can show up as a dry, tickling cough or a wet, productive one that brings up mucus. Knowing the difference matters more than most people think, because the best treatment for each type isn’t the same.
Dry Cough vs. Productive Cough
A dry cough produces no mucus. It often results from viral infections, allergies, acid reflux, or irritants like smoke and dust. That persistent tickle in your throat? It can wreck your sleep and make it hard to concentrate during the day.
A productive (wet) cough brings up phlegm or mucus from your lungs and airways. This type usually signals a chest cold, bronchitis, or sinus drainage. And here’s the thing: productive coughs actually serve a purpose. They help your body clear out infection and debris. So suppressing them isn’t always the right call.
Acute vs. Chronic Cough
An acute cough lasts less than three weeks. The most common cause? A plain old cold. According to the Mayo Clinic, most acute coughs resolve on their own within 7 to 10 days.
A chronic cough persists beyond eight weeks in adults (four weeks in children). Common causes include asthma, postnasal drip, gastroesophageal reflux disease (GERD), and certain medications like ACE inhibitors. If you’ve been coughing for two months straight, don’t just keep reaching for lozenges. Get it evaluated.
Best Natural Cough Remedies
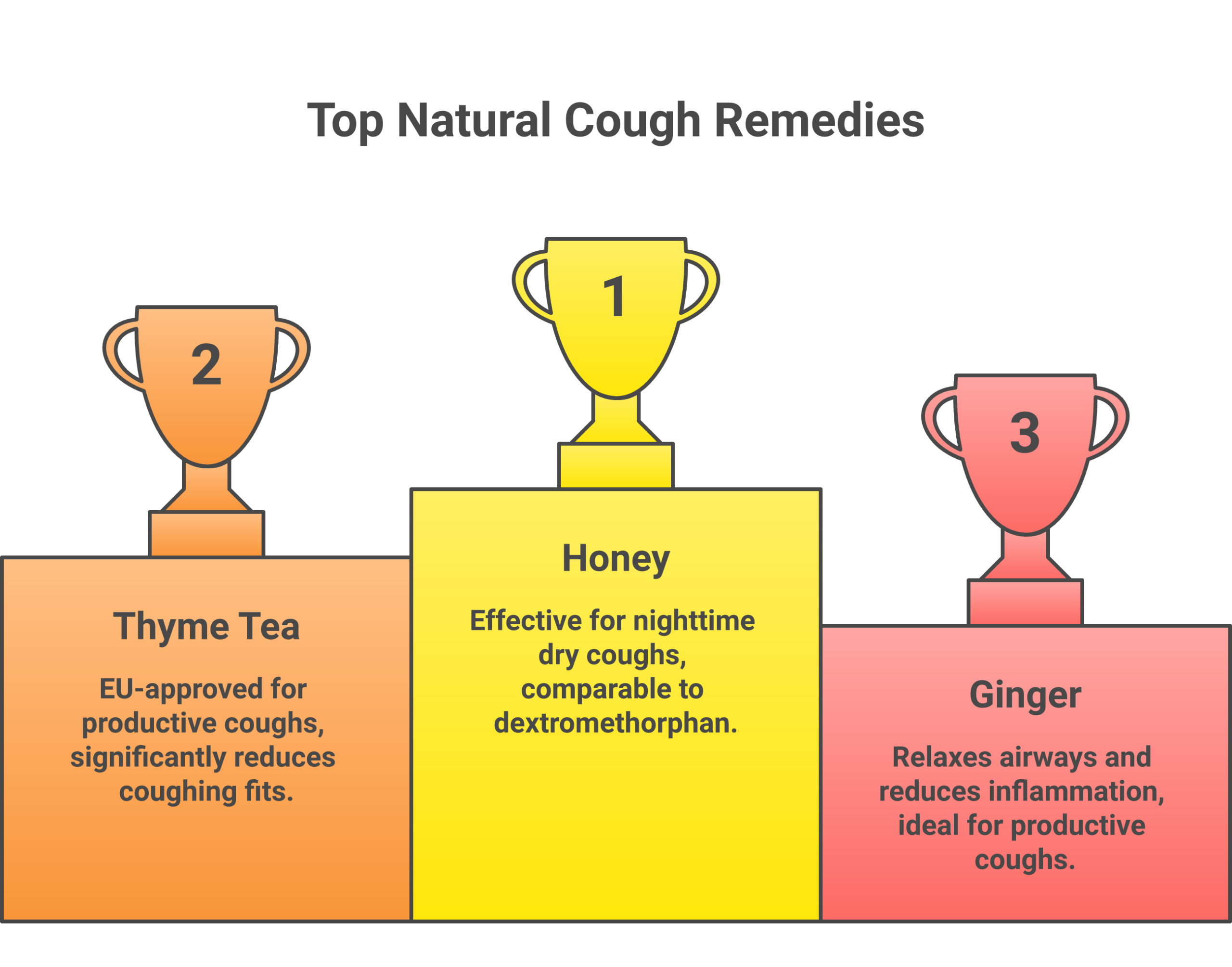
Natural remedies work best for acute coughs caused by colds and mild respiratory infections. I’ve organized these by strength of evidence, starting with the one that has the most clinical research behind it.
Honey
Honey is, hands down, the most underrated cough remedy out there. People dismiss it as a folk cure, but the research tells a different story.
A 2018 Cochrane review of six randomized controlled trials involving 899 children found that honey probably reduces cough symptoms more than placebo and is likely more effective at relieving nighttime cough than no treatment (Oduwole et al., Cochrane Database of Systematic Reviews, 2018). The review also found little or no difference between honey and dextromethorphan for overall cough relief. Read that again: honey matched a pharmaceutical cough suppressant in head-to-head trials.
A separate 2021 systematic review and meta-analysis in BMJ Evidence-Based Medicine (Abuelgasim, Albury, and Lee) analyzed 14 studies and found honey reduced cough frequency by a standardized mean difference of -0.36 compared to standard care.
How to take it: 1 to 2 teaspoons of raw honey straight, or stir it into warm water or herbal tea. Works best right before bedtime for nighttime coughs. One important warning: never give honey to children under 12 months due to the risk of infant botulism.
Thyme Tea
Thyme (Thymus vulgaris) has antispasmodic and expectorant properties, and there’s actual trial data to back it up.
A 2006 double-blind, placebo-controlled trial published in Arzneimittelforschung (Kemmerich et al.) tested a thyme-ivy fluid extract combination in adults with acute bronchitis. Coughing fits dropped by 68.7% in the thyme group versus 47.6% with placebo over days 7 to 9. The 50% reduction milestone was reached two days earlier with thyme. The European Medicines Agency has approved thyme-based preparations as traditional herbal medicines for productive cough associated with the common cold.
Preparation: Steep 2 teaspoons of dried thyme in 8 ounces of boiling water for 10 minutes. Strain and drink up to three cups per day. Adding honey gives you a two-for-one benefit.
Marshmallow Root
Marshmallow root (Althaea officinalis) contains mucilage, a gel-like substance that coats and soothes irritated throat tissue. If you’ve got a dry, scratchy cough that won’t quit, this one’s worth trying.
A 2018 survey-based study published in Complementary Medicine Research (Fasse et al.) found that participants reported both marshmallow root lozenges and syrup helped relieve dry cough. The mucilage creates a protective film over the throat lining, which reduces the cough reflex triggered by irritation. A separate in vitro study in Frontiers in Pharmacology (2020) confirmed anti-inflammatory and antioxidant effects on airway cells.
Preparation: Make a cold infusion by soaking 1 tablespoon of dried marshmallow root in 1 cup of cold water for 1 to 2 hours, then strain. You can also find marshmallow root lozenges and syrups at most health food stores.
Ginger
Ginger contains compounds called gingerols and shogaols that relax airway smooth muscles, according to a 2013 study in the American Journal of Respiratory Cell and Molecular Biology. That relaxation effect can help calm coughs triggered by bronchospasm. Ginger’s also got anti-inflammatory properties that soothe an irritated throat.
Slice about an inch of fresh ginger root and steep it in hot water for 10 to 15 minutes. Add honey and lemon. Two to 3 cups daily works well, and it’s particularly useful for productive coughs because ginger may help thin mucus.
Peppermint
Peppermint contains menthol, a natural decongestant. That cooling sensation you feel? It temporarily opens nasal passages and soothes throat irritation. The American Lung Association lists peppermint tea among helpful remedies for managing cough symptoms at home. Menthol is also the active ingredient in many OTC cough drops and throat lozenges, so you’ve probably used it without realizing.
Brew peppermint tea, or add 3 to 4 drops of peppermint essential oil to a bowl of hot water for steam inhalation. Don’t apply peppermint oil directly to skin without diluting it, and avoid using it around infants and young children.
Steam Inhalation
Breathing in warm, moist air loosens mucus in your nasal passages and chest. Simple, cheap, and it works fast. A humidifier or a bowl of steaming water does the job. The Mayo Clinic Health System recommends a cool-mist vaporizer or humidifier to add moisture to your home when you’re dealing with cough and cold symptoms.
Fill a bowl with hot (not boiling) water. Drape a towel over your head, lean over the bowl, and breathe deeply for 5 to 10 minutes. A few drops of eucalyptus oil is optional but can enhance the decongestant effect. Steam’s especially helpful when you’ve got thick chest congestion.
Saltwater Gargle
Old-school and effective. Gargling with warm salt water draws moisture out of swollen throat tissues, reducing inflammation and loosening mucus. The Mayo Clinic includes saltwater gargles in its list of cold remedies that may help relieve symptoms.
Dissolve 1/4 to 1/2 teaspoon of table salt in 8 ounces of warm water. Gargle for 15 to 30 seconds, then spit. Repeat several times per day as needed. Not recommended for children under 6, though, since they often can’t gargle without swallowing.
If you’re looking for cough supplements that combine several of these ingredients, our review team has evaluated the top products on the market.
Best OTC Cough Suppressants and Expectorants
When natural remedies aren’t cutting it, OTC cough medications can provide stronger relief. There are two main categories: suppressants (antitussives) and expectorants. Which one you want depends on whether your cough is dry or productive.
Dextromethorphan (Cough Suppressant)
Dextromethorphan (DXM) is the most widely used OTC cough suppressant. It acts on the cough center in your brain to reduce the urge to cough. A review published by the American Academy of Family Physicians found that a single 30-mg dose was more effective than placebo at reducing cough frequency and intensity in adult studies. You’ll find it in Robitussin DM and Delsym, among others.
Best for: Dry, non-productive coughs that keep you up at night or interfere with your day.
Dosage (adults): 10 to 20 mg every 4 hours, or 30 mg every 6 to 8 hours, as directed on the label. Don’t exceed 120 mg in 24 hours.
Side effects: Drowsiness, dizziness, and nausea at recommended doses. DXM has potential for misuse at high doses, which the FDA has specifically flagged.
Guaifenesin (Expectorant)
Guaifenesin is the only FDA-approved OTC expectorant medicine for mucus. It thins and loosens mucus in your airways, making it easier to cough up. Mucinex is the most recognized brand.
The evidence is decent but not airtight. A review in Pulmonary Pharmacology and Therapeutics (2017) found that four of five large-scale trials showed significant improvements in cough frequency, intensity, and mucus thickness with guaifenesin compared to placebo. But a 2013 study in Respiratory Research found no measurable effect on sputum volume or properties. So results can vary.
Best for: Productive (wet) coughs with thick mucus or chest congestion.
Dosage (adults): 200 to 400 mg every 4 hours, as directed. Drink plenty of water when taking guaifenesin to help loosen mucus.
Important note: Avoid suppressing a productive cough completely. Coughing up mucus helps clear infection from your lungs. If you’ve got a wet cough, an expectorant is almost always a better choice than a suppressant.
For a closer look at top cough suppressant products with expert analysis, see our cough supplement reviews.
Honey as a Cough Suppressant: What Research Shows
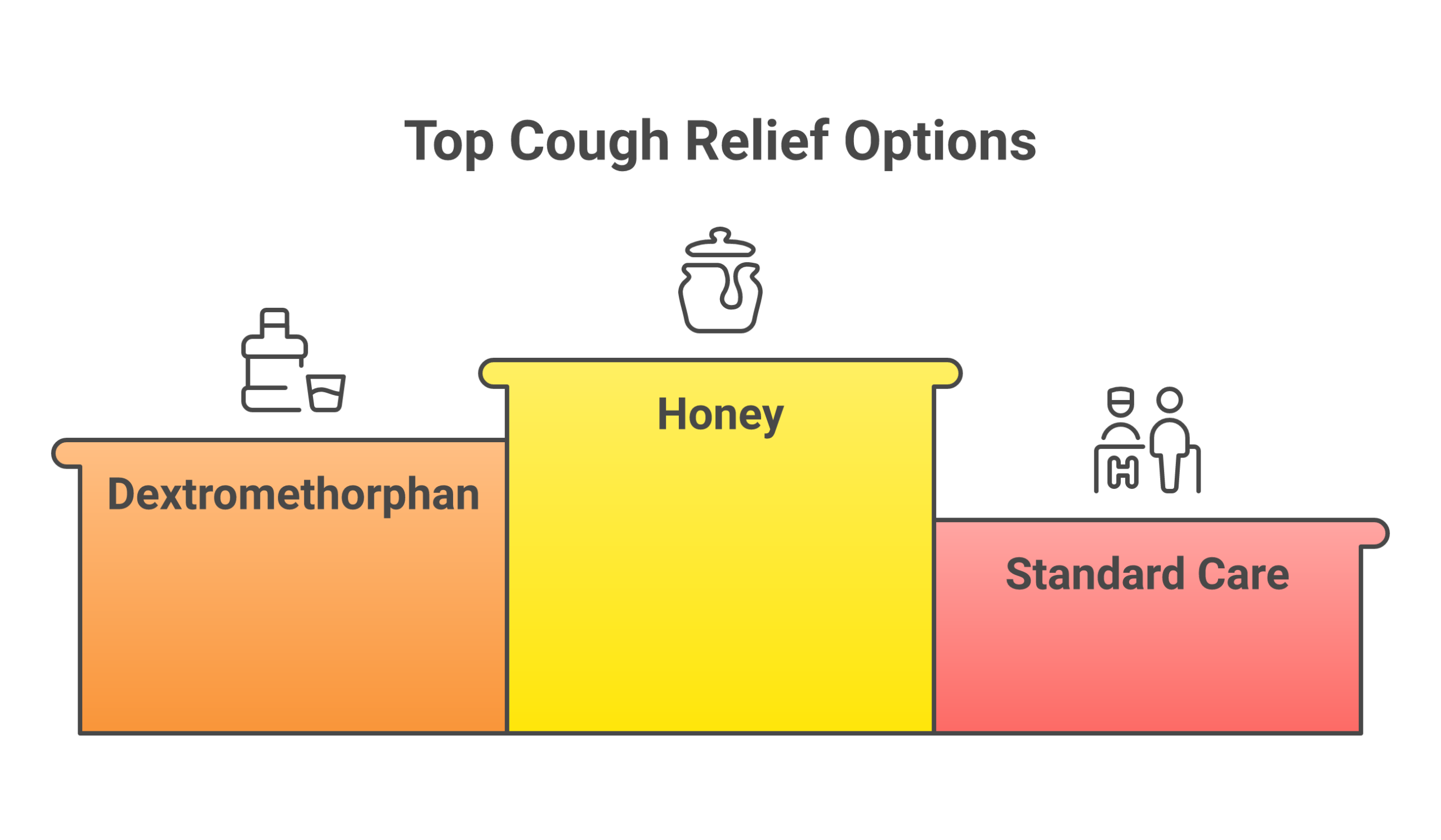
Honey deserves its own section because the clinical evidence is stronger than most people realize. It’s not a folk remedy with wishful thinking behind it. Multiple randomized controlled trials have tested honey head-to-head against pharmaceutical cough suppressants, and the results surprised a lot of people.
The most rigorous evidence comes from the 2018 Cochrane review (Oduwole et al.), which pooled data from six RCTs and 899 children. The review concluded that honey “probably reduces cough symptoms more than placebo” and performs comparably to dextromethorphan.
Then there’s the 2007 study in Archives of Pediatrics and Adolescent Medicine (Paul et al.) that compared buckwheat honey, honey-flavored DXM, and no treatment in 105 children ages 2 to 18. Parents rated buckwheat honey highest for cough frequency reduction, cough severity, and sleep quality improvement. That’s buckwheat honey beating a pharmaceutical in a controlled trial.
The 2021 BMJ meta-analysis (Abuelgasim et al.) extended these findings to adults. Across 14 studies, honey reduced combined symptom scores by a mean difference of -3.96 compared to standard care. The authors called honey “a widely available and cheap alternative to antibiotics” for upper respiratory symptoms, and noted it should be recommended before prescribing antibiotics for mild infections.
Why does honey work? Researchers believe the thick consistency coats and soothes irritated throat tissue. The natural sugars may trigger saliva production and airway secretions, which help thin mucus. Honey also has antimicrobial properties. Dark varieties like buckwheat and manuka tend to have higher antioxidant content.
Safety limits: Never give honey to children under 12 months (botulism risk). For adults and older children, 1 to 2 teaspoons before bed is the standard dose used in clinical trials. One thing to keep in mind: long-term nightly use could contribute to dental issues, so it’s not meant as an indefinite solution.
Looking for healthy cough syrup alternatives that pair honey with other natural ingredients? Browse our cough and respiratory supplement category for options reviewed by our editorial team.
When to See a Doctor
Most acute coughs clear up within one to three weeks on their own. But some symptoms are red flags. See a doctor if you experience any of these:
- Cough lasting longer than 3 weeks with no improvement
- Coughing up blood or blood-tinged mucus
- Fever above 103 degrees Fahrenheit (39.4 degrees Celsius) that won’t break
- Shortness of breath or difficulty breathing
- Chest pain not related to the act of coughing itself
- Wheezing or a whistling sound when you breathe
- Unexplained weight loss alongside a persistent cough
- Worsening symptoms after you started getting better (could indicate a secondary bacterial infection)
According to the Cleveland Clinic, productive coughs that worsen over time or produce yellow-green, thick mucus may indicate bronchitis or pneumonia, both of which may require prescription antibiotics or other treatments.
For people with nerve-related discomfort or chronic conditions, persistent coughing can aggravate existing symptoms. Our resource on vitamins and supplements for nerve regeneration covers supportive nutrients that may help with overall recovery.
Natural Cough Remedies for Children
Children’s coughs need a different approach, and this is one area where being cautious really matters. The FDA and the American Academy of Pediatrics (AAP) recommend against giving OTC cough and cold medicines to children under 4 years old. For children ages 4 to 6, only use these medicines if a pediatrician specifically says to.
Safe Options by Age
Children under 12 months: Your options are limited, but they work. Offer small amounts of clear fluids (water, diluted juice) to keep the throat moist. Use a cool-mist humidifier in the bedroom. Saline nose drops and gentle bulb syringe suctioning can help with nasal congestion that triggers coughing.
Children ages 1 to 5: This is where honey becomes your best friend. It’s safe starting at age 1. Give 1/2 to 1 teaspoon as needed, especially before bedtime. The 2018 Cochrane review confirmed that honey likely reduces cough symptoms in this age group. Keep the humidifier running and push fluids.
Children ages 6 and older: All of the natural remedies listed above are generally safe at this age. Honey (1 to 2 teaspoons), warm teas, steam inhalation (with supervision), and saltwater gargles all work. OTC medications may be appropriate too, but always follow label dosing and check with a pharmacist if you’re unsure about interactions.
What to Avoid
- Honey for infants under 12 months (botulism risk)
- OTC cough medicines for children under 4 (per FDA guidance)
- Codeine-containing products for anyone under 18 (FDA issued a black-box warning in 2018 due to risk of slowed or difficult breathing)
- Eucalyptus and peppermint essential oils on young children’s faces (can cause breathing difficulty in infants)
If your child’s cough comes with high fever, rapid breathing, or blue-tinged lips, get to an emergency room. Don’t wait for a regular appointment. Those could be signs of pneumonia or another serious respiratory condition.
Parents managing multiple health concerns can also explore our guides to supplements for digestive health and gut health supplements for a broader approach to children’s wellness.
Frequently Asked Questions
What is the best medicine for a bad cough?
It depends on the type of cough. For a dry cough, dextromethorphan (found in Robitussin DM, Delsym) is the most common OTC suppressant. For a wet, productive cough with mucus, guaifenesin (Mucinex) is the standard expectorant medicine for mucus. For a natural alternative, the 2018 Cochrane review found honey performs comparably to dextromethorphan in reducing cough symptoms.
Does honey actually work for cough?
Yes. A 2021 systematic review in BMJ Evidence-Based Medicine analyzed 14 studies and found honey reduced cough frequency and severity compared to standard care. It also matched dextromethorphan’s effectiveness in a 2018 Cochrane review of 899 children. Take 1 to 2 teaspoons of raw honey before bed. Don’t give honey to children under 12 months.
What is a healthy cough syrup alternative?
Honey mixed with warm water or herbal tea (thyme, ginger, or peppermint) is the most studied healthy cough syrup option. Marshmallow root syrup is another option for dry, irritating coughs because its mucilage coats the throat. For curated product recommendations, visit our cough supplement review page.
Can I take a cough suppressant and expectorant together?
Yes. Many combination products (like Mucinex DM) contain both guaifenesin and dextromethorphan. The expectorant thins mucus while the suppressant reduces coughing frequency. This combination is considered safe for adults when taken as directed. Consult your pharmacist if you’re taking other medications.
How long should a cough last before I see a doctor?
See a doctor if your cough lasts longer than three weeks, produces blood or blood-tinged mucus, is accompanied by a fever above 103 degrees Fahrenheit, or makes it hard to breathe. The Cleveland Clinic advises that worsening coughs with thick, colored mucus may signal bronchitis or pneumonia.
Are OTC cough medicines safe for children?
The FDA recommends against giving OTC cough and cold medicines to children under 4 years old. For children ages 4 to 6, use them only with a doctor’s guidance. Honey (for children 1 and older) and humidified air are the safest first-line options for young children. Codeine-containing cough products shouldn’t be given to anyone under 18.
What natural remedies help with mucus and chest congestion?
Steam inhalation, warm fluids, ginger tea, and guaifenesin are all effective for loosening thick mucus. Thyme tea has expectorant properties backed by clinical trials. But honestly, the single most important thing you can do for mucus is stay hydrated. Drinking enough water thins mucus and makes productive coughs more effective at clearing your airways.
Medical Disclaimer: This article is for informational purposes only and does not constitute medical advice. The content on Consumer Health Guide is not intended to be a substitute for professional medical diagnosis, treatment, or guidance. Always consult a qualified healthcare provider before starting any new supplement, herbal remedy, or medication, especially for children, pregnant or nursing women, and individuals with pre-existing medical conditions. If you are experiencing severe or persistent symptoms, seek medical attention promptly. Individual results may vary. The information presented here reflects published clinical research and official medical guidelines as of March 2026.
Last updated: March 26, 2026 | Medically reviewed content | Consumer Health Guide | About Our Review Process

